Abstract
Purpose
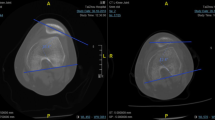
Management of post-traumatic patellar instability in children with osseous abnormalities is challenging because of the presence of an open physis. The aim of our study was to compare the rate of recurrence after isolated reconstruction of the medial patellofemoral ligament (MPFL) in children with or without osseous abnormalities.
Methods
The medical records of 25 children (27 knees) with recurrent patellar dislocation were reviewed. Each child underwent an isolated reconstruction of the MPFL using a hamstring graft. At the last follow-up, a clinical and radiographic evaluation was performed, including assessment of functional outcomes based on the Kujala score. Patients were compared in terms of the occurrence of a pre-existing osseous abnormality.
Results
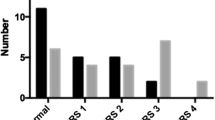
The mean age at the time of the surgery was 13.8 years. Eleven patients had trochlear dysplasia (40%), three had a patella alta (11%) and seven had an increased TT-TG (26%). The recurrence rate was 3.7% (one patient), after a mean follow-up of 41.1 months. Recurrence was not more frequent in patients with preoperative anatomical predisposing factors. The mean Kujala score was 95. The mean time to return to practicing sports was 7.1 months.
Conclusions
Isolated MPFL reconstruction is an effective option for the management of post-traumatic patellofemoral instability in skeletally immature patients. The results of this technique seem to be independent on either proximal or distal misalignments such as trochlear dysplasia, patella alta, or increased TT-TG.


Similar content being viewed by others
References
Zaidi A, Babyn P, Astori I et al (2006) MRI of traumatic patellar dislocation in children. Pediatr Radiol 36:1163–1170. https://doi.org/10.1007/s00247-006-0293-0
Kepler CK, Bogner E a, Hammoud S et al (2011) Zone of injury of the medial patellofemoral ligament after acute patellar dislocation in children and adolescents. Am J Sports Med 39:1444–1449. https://doi.org/10.1177/0363546510397174
Askenberger M, Arendt EA, Ekstro m W et al (2016) Medial patellofemoral ligament injuries in children with first-time lateral patellar dislocations: a magnetic resonance imaging and arthroscopic study. Am J Sports Med 44:152–158. https://doi.org/10.1177/0363546515611661
Petri M, von Falck C, Broese M et al (2013) Influence of rupture patterns of the medial patellofemoral ligament (MPFL) on the outcome after operative treatment of traumatic patellar dislocation. Knee Surg Sport Traumatol Arthrosc 21:683–689. https://doi.org/10.1007/s00167-012-2037-z
Desio SM, Burks RT, Bachus KN (1998) Soft tissue restraints to lateral patellar translation in the human knee. Am J Sports Med 26:59–65. https://doi.org/10.1177/03635465980260012701
Wilson A, Afarin A, Shaw C et al (2013) Magnetic resonance imaging findings after acute patellar dislocation in children. Orthop J Sport Med 1:2325967113512460. https://doi.org/10.1177/2325967113512460
Lind M, Enderlein D, Nielsen T et al (2016) Clinical outcome after reconstruction of the medial patellofemoral ligament in paediatric patients with recurrent patella instability. Knee Surg Sport Traumatol Arthrosc 24:666–671. https://doi.org/10.1007/s00167-014-3439-x
Nwachukwu BU, So C, Schairer WW et al (2016) Surgical versus conservative management of acute patellar dislocation in children and adolescents: a systematic review. Knee Surg Sports Traumatol Arthrosc 24:760–767. https://doi.org/10.1007/s00167-015-3948-2
Dejour H, Walch G, Nove-Josserand L, Guier C (1994) Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 2:19–26
Hopper GP, Leach WJ, Rooney BP et al (2014) Does degree of trochlear dysplasia and position of femoral tunnel influence outcome after medial patellofemoral ligament reconstruction? Am J Sports Med 42:716–722. https://doi.org/10.1177/0363546513518413
Crosby EB, Insall J (1976) Recurrent dislocation of the patella. Relation of treatment to osteoarthritis. J Bone Joint Surg Am 58:9–13
Sillanpää P, Mattila VM, Visuri T et al (2008) Ligament reconstruction versus distal realignment for patellar dislocation. Clin Orthop Relat Res 466:1475–1484. https://doi.org/10.1007/s11999-008-0207-6
Pesenti S, Blondel B, Armaganian G, et al (2016) The lateral wedge augmentation trochleoplasty in a pediatric population. J Pediatr Orthop B 1. doi: https://doi.org/10.1097/BPB.0000000000000395
Davis IS (2011) Landing pattern modification to improve patellofemoral pain in runners: a case series. J Orthop Sports Phys Ther 41:914–919. https://doi.org/10.2519/jospt.2011.3771
Trentacosta NE, Vitale MA, Ahmad CS (2009) The effects of timing of pediatric knee ligament surgery on short-term academic performance in school-aged athletes. Am J Sports Med 37:1684–1691. https://doi.org/10.1177/0363546509332507
Nelitz M, Dreyhaupt J, Reichel H et al (2013) Anatomic reconstruction of the medial patellofemoral ligament in children and adolescents with open growth plates: surgical technique and clinical outcome. Am J Sports Med 41:58–63. https://doi.org/10.1177/0363546512463683
Vavken P, Wimmer MD, Camathias C et al (2013) Treating patella instability in skeletally immature patients. Arthroscopy 29:1410–1422. https://doi.org/10.1016/j.arthro.2013.03.075
Malecki K, Fabis J, Flont P et al (2016) Preliminary results of two surgical techniques in the treatment of recurrent patellar dislocation: medial patellofemoral ligament reconstruction versus combined technique of vastus medialis advancement, capsular plasty and roux-Goldthwait procedure in tr. Int Orthop 40:1869–1874. https://doi.org/10.1007/s00264-016-3119-1
Fabricant PD, Ladenhauf HN, Salvati EA, Green DW (2014) Medial patellofemoral ligament (MPFL) reconstruction improves radiographic measures of patella alta in children. Knee 21:1180–1184. https://doi.org/10.1016/j.knee.2014.07.023
Ostermeier S, Stukenborg-Colsman C, Hurschler C, Wirth C-J (2006) In vitro investigation of the effect of medial patellofemoral ligament reconstruction and medial tibial tuberosity transfer on lateral patellar stability. Arthroscopy 22:308–319. https://doi.org/10.1016/j.arthro.2005.09.024
Mani S, Kirkpatrick MS, Saranathan A et al (2011) Tibial tuberosity osteotomy for patellofemoral realignment alters tibiofemoral kinematics. Am J Sports Med 39:1024–1031. https://doi.org/10.1177/0363546510390188
Kita K, Tanaka Y, Toritsuka Y et al (2015) Factors affecting the outcomes of double-bundle medial patellofemoral ligament reconstruction for recurrent patellar dislocations evaluated by multivariate analysis. Am J Sports Med 43:2988–2996. https://doi.org/10.1177/0363546515606102
Clark D, Metcalfe A, Wogan C et al (2017) Adolescent patellar instability. Bone Joint J 99–B:159–170. https://doi.org/10.1302/0301-620X.99B2.BJJ-2016-0256.R1
Ambrožič B, Novak S (2016) The influence of medial patellofemoral ligament reconstruction on clinical results and sports activity level. Phys Sportsmed 44:133–140. https://doi.org/10.1080/00913847.2016.1148561
Tompkins MA, Arendt EA (2015) Patellar instability factors in isolated medial patellofemoral ligament reconstructions--what does the literature tell us? A systematic review. Am J Sports Med 43:2318–2327. https://doi.org/10.1177/0363546515571544
Acknowledgments
SP received grants from the Société Française de Chirurgie Orthopédique et Traumatologie (SOFCOT) and from the Société Française de Chirurgie Orthopédique Pédiatrique (SOFOP) and from the Association pour le Développement de la Recherche Médicale (ADEREM).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors declare any conflict of interest.
Additional information
Level of evidence: IV, case series
Rights and permissions
About this article
Cite this article
Pesenti, S., Ollivier, M., Escudier, JC. et al. Medial patellofemoral ligament reconstruction in children: do osseous abnormalities matter?. International Orthopaedics (SICOT) 42, 1357–1362 (2018). https://doi.org/10.1007/s00264-017-3750-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-017-3750-5