Abstract
Purpose
Female patients with pelvic floor diseases may suffer from several sexual disorders and sexual life impairments. The aim of this manuscript was to evaluate sexual dysfunction in female patients presenting with faecal incontinence (FI) and defecation disorder (DD).
Methods
A retrospective review was performed of a prospectively collected database of sexually active women referred to the pelvic floor clinic, who completed the Pelvic Organ Prolapse/Incontinence Sexual Questionnaire-12 (PISQ-12) at first visit. Statistical analysis was performed to evaluate and compare sexual dysfunction between patients with FI and DD and with published data on the general population. Regression analysis was used to identify predictors of sexual dysfunction and surgery.
Results
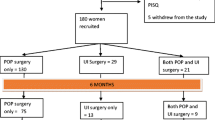
Three hundred thirteen patients were included, 192 (61%) with FI and 121 (39%) with DD. The patients with DD received more non-gynaecological surgical procedures (p = 0.023). More patients with DD received surgery for their current pelvic floor disease (p < 0.001). Major sexual impairment (PISQ-12 < 30) was found in 100 patients (31.9%). The mean PISQ-12 (33.2 ± 7.2) score was by 5 points lower than those reported in the general population from PISQ-validating studies. Prior anorectal surgery (odds ratio (OR) = 15.4), partner ejaculation problems (PISQ item 11, OR = 2.5), reduced sexual arousal (item 2, OR = 2.1), and orgasm perception (item 13, OR = 2.1) were the strongest predictors of worse sexual function in patients with FI. Patients with DD were almost 15 times more likely to receive subsequent surgery (OR = 14.6, p < 0.001), whereas fear of urine leakage almost doubled the risk.
Conclusions
Sexual dysfunction is prevalent among patients suffering from FI and DD, and questionnaires are useful in recognizing these patients. Subsequent surgery is more common for patients with DD compared to those with FI.


Similar content being viewed by others
References
Spector IP, Carey MP (1990) Incidence and prevalence of the sexual dysfunctions: a critical review of the empirical literature. Arch Sex Behav 19(4):389–408
Panman CM, Wiegersma M, Talsma MN, Kollen BJ, Berger MY, Lisman-Van Leeuwen Y, Dekker JH (2014) Sexual function in older women with pelvic floor symptoms: a cross-sectional study in general practice. Br J Gen Pract 64(620):e144–e150. doi:10.3399/bjgp14X677518
Cichowski SB, Komesu YM, Dunivan GC, Rogers RG (2013) The association between fecal incontinence and sexual activity and function in women attending a tertiary referral center. Int Urogynecol J 24(9):1489–1494. doi:10.1007/s00192-013-2044-8
Rogers RG, Coates KW, Kammerer-Doak D, Khalsa S, Qualls C (2003) A short form of the Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire (PISQ-12). Int Urogynecol J Pelvic Floor Dysfunct 14(3):164–168 . doi:10.1007/s00192-003-1063-2discussion 168
Haylen BT, Maher CF, Barber MD, Camargo S, Dandolu V, Digesu A, Goldman HB, Huser M, Milani AL, Moran PA, Schaer GN, Withagen MI (2016) An International Urogynecological Association (IUGA) / International Continence Society (ICS) joint report on the terminology for female pelvic organ prolapse (POP). Int Urogynecol J 27(2):165–194. doi:10.1007/s00192-015-2932-1
Mamik MM, Rogers RG, Qualls CR, Morrow JD (2014) The minimum important difference for the Pelvic Organ Prolapse-Urinary Incontinence Sexual Function Questionnaire. Int Urogynecol J 25(10):1321–1326. doi:10.1007/s00192-014-2342-9
Shaaban MM, Abdelwahab HA, Ahmed MR, Shalaby E (2014) Assessment of female sexual function among women with pelvic organ prolapse or urinary incontinence via an Arabic validated short-form sexual questionnaire. Int J Gynaecol Obstet 124(1):24–26. doi:10.1016/j.ijgo.2013.06.031
Santana GW, Aoki T, Auge AP (2012) The Portuguese validation of the short form of the Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire (PISQ-12). Int Urogynecol J 23(1):117–121. doi:10.1007/s00192-011-1505-1
Lowenstein L, Pierce K, Pauls R (2009) Urogynecology and sexual function research. How are we doing? J Sex Med 6(1):199–204. doi:10.1111/j.1743-6109.2008.00968.x
Chandraiah S, Levenson JL, Collins JB (1991) Sexual dysfunction, social maladjustment, and psychiatric disorders in women seeking treatment in a premenstrual syndrome clinic. Int J Psychiatry Med 21(2):189–204
Read S, King M, Watson J (1997) Sexual dysfunction in primary medical care: prevalence, characteristics and detection by the general practitioner. J Public Health Med 19(4):387–391
Líndal E, Stefànsson JG (1993) The lifetime prevalence of psychosexual dysfunction among 55 to 57-year-olds in Iceland. Soc Psychiatry Psychiatr Epidemiol 28(2):91–95
Moody GA, Mayberry JF (1993) Perceived sexual dysfunction amongst patients with inflammatory bowel disease. Digestion 54(4):256–260
Pauls RN, Rogers RG, Parekh M, Pitkin J, Kammerer-Doak D, Sand P (2015) Sexual function in women with anal incontinence using a new instrument: the PISQ-IR. Int Urogynecol J 26(5):657–663. doi:10.1007/s00192-014-2563-y
Shimonov M, Groutz A, Schachter P, Gordon D (2015) Is bariatric surgery the answer to urinary incontinence in obese women? Neurourol Urodyn. doi:10.1002/nau.22909
Ramage L, Georgiou P, Tekkis P, Tan E (2015) Is robotic ventral mesh rectopexy better than laparoscopy in the treatment of rectal prolapse and obstructed defecation? A meta-analysis. Techniques in coloproctology 19(7):381–389. doi:10.1007/s10151-015-1320-7
Meriwether KV, Komesu YM, Craig E, Qualls C, Davis H, Rogers RG (2015) Sexual function and pessary management among women using a pessary for pelvic floor disorders. J Sex Med 12(12):2339–2349. doi:10.1111/jsm.13060
Thibault F, Costa P, Thanigasalam R, Seni G, Brouzyine M, Cayzergues L, De Tayrac R, Droupy S, Wagner L (2013) Impact of laparoscopic sacrocolpopexy on symptoms, health-related quality of life and sexuality: a medium-term analysis. BJU Int 112(8):1143–1149. doi:10.1111/bju.12286
Simons JS, Carey MP (2001) Prevalence of sexual dysfunctions: results from a decade of research. Arch Sex Behav 30(2):177–219
Botros SM, Abramov Y, Miller JJ, Sand PK, Gandhi S, Nickolov A, Goldberg RP (2006) Effect of parity on sexual function: an identical twin study. Obstet Gynecol 107(4):765–770. doi:10.1097/01.AOG.0000207677.03235.76
Cetinkaya SE, Dokmeci F, Dai O (2013) Correlation of pelvic organ prolapse staging with lower urinary tract symptoms, sexual dysfunction, and quality of life. Int Urogynecol J 24(10):1645–1650. doi:10.1007/s00192-013-2072-4
Collins SA, O‘Sullivan DM, LaSala CA (2010) Factors associated with PISQ-12 completion in an academic urogynecology population. Int Urogynecol J 21(5):579–582. doi:10.1007/s00192-009-1079-3
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
For this type of study, formal consent is not required.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
The abstract of this manuscript was accepted as a Lunchtime Poster at the ESCP 11th Scientific & Annual Meeting, Milan, September 28–30, 2016.
Rights and permissions
About this article
Cite this article
Pellino, G., Ramage, L., Simillis, C. et al. Evaluation of sexual dysfunction in female patients presenting with faecal incontinence or defecation disorder. Int J Colorectal Dis 32, 667–674 (2017). https://doi.org/10.1007/s00384-017-2795-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-017-2795-7