Abstract
Purpose
Obstructive sleep apnea (OSA) is underdiagnosed in females due to different clinical presentation. We aimed to determine the effect of gender on clinical and polysomnographic features and identify predictors of OSA in women.
Methods
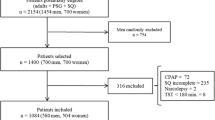
Differences in demographic, clinical, and polysomnographic parameters between 2052 male and 775 female OSA patients were compared.
Results
In female OSA patients, age (56.1 ± 9.7 vs. 50.4 ± 11.6 years, p < 0.0001) and body mass index (36.3 ± 8.6 vs. 31.8 ± 5.9 kg/m2, p < 0.0001) were increased, whereas men had higher waist-to-hip ratio and neck circumference (p < 0.0001). Hypertension, diabetes mellitus, thyroid disease, and asthma were more common in females (p < 0.0001). Men reported more witnessed apnea (p < 0.0001), but nocturnal choking, morning headache, fatigue, insomnia symptoms, impaired memory, mood disturbance, reflux, nocturia, and enuresis were more frequent in women (p < 0.0001).
The indicators of OSA severity including apnea-hypopnea index (AHI) (p < 0.0001) and oxygen desaturation index (p = 0.007) were lower in women. REM AHI (p < 0.0001) was higher, and supine AHI (p < 0.0001) was lower in females. Besides, women had decreased total sleep time (p = 0.028) and sleep efficiency (p = 0.003) and increased sleep latency (p < 0.0001). In multivariate logistic regression analysis, increased REM AHI, N3 sleep, obesity, age, morning headache, and lower supine AHI were independently associated with female gender.
Conclusions
These data suggest that frequency and severity of sleep apnea is lower in female OSA patients, and they are presenting with female-specific symptoms and increased medical comorbidities. Therefore, female-specific questionnaires should be developed and used for preventing underdiagnosis of OSA.


Similar content being viewed by others
Abbreviations
- AHI:
-
apnea-hypopnea index
- BMI:
-
body mass index
- CI:
-
confidence interval
- CPAP:
-
continuous positive airway pressure
- ESS:
-
Epworth sleepiness score
- FEV1 :
-
forced expiratory volume in one second
- FVC:
-
forced vital capacity
- N:
-
non-rapid eye movement
- ODI:
-
oxygen desaturation index
- OR:
-
odds ratio
- OSA:
-
obstructive sleep apnea
- PaCO2 :
-
arterial partial pressure of carbon dioxide
- PaO2 :
-
arterial partial pressure of oxygen
- REM:
-
rapid eye movement
- SWS:
-
slow wave sleep
- SpO2 :
-
oxygen saturation
References
Franklin KA, Lindberg E (2015) Obstructive sleep apnea is a common disorder in the population—a review on the epidemiology of sleep apnea. J Thorac Dis 7:1311–1322
Lévy P, Ryan S, Oldenburg O, Parati G (2013) Sleep apnoea and the heart. Eur Respir Rev 22:333–352
Selim B, Won C, Yaggi HK (2010) Cardiovascular consequences of sleep apnea. Clin Chest Med 31:203–220
Lyons OD, Ryan CM (2015) Sleep apnea and stroke. Can J Cardiol 31:918–927
Bonsignore MR, Borel AL, Machan E, Grunstein R (2013) Sleep apnoea and metabolic dysfunction. Eur Respir Rev 22:353–364
Kent BD, McNicholas WT, Ryan S (2015) Insulin resistance, glucose intolerance and diabetes mellitus in obstructive sleep apnoea. J Thorac Dis 7:1343–1357
Ye L, Pien GW, Weaver TE (2009) Gender differences in the clinical manifestation of obstructive sleep apnea. Sleep Med 10:1075–1084
Jordan AS, McEvoy RD (2003) Gender differences in sleep apnea: epidemiology, clinical presentation and pathogenic mechanisms. Sleep Med Rev 7:377–389
Valipour A (2012) Gender-related differences in the obstructive sleep apnea syndrome. Pneumologie 66:584–588
Ralls FM, Grigg-Damberger M (2012) Roles of gender, age, race/ethnicity, and residential socioeconomics in obstructive sleep apnea syndromes. Curr Opin Pulm Med 18:568–573
Saaresranta T, Anttalainen U, Polo O (2015) Sleep disordered breathing: is it different for females? ERJ Open Res 1:00063–02015
Yamakoshi S, Kasai T, Tomita Y, Takaya H, Kasagi S, Kawabata M et al (2016) Comparison of clinical features and polysomnographic findings between men and women with sleep apnea. J Thorac Dis 8:145–151
Vagiakis E, Kapsimalis F, Lagogianni I, Perraki H, Minaritzoglou A, Alexandropoulou K et al (2006) Gender differences on polysomnographic findings in Greek subjects with obstructive sleep apnea syndrome. Sleep Med 7:424–430
Izci B, Ardic S, Firat H, Sahin A, Altinors M, Karacan I (2008) Reliability and validity studies of the Turkish version of the Epworth Sleepiness Scale. Sleep Breath 12:161–168
Iber C, Ancoli-Israel S, Chesson AL (2007) In: Quan SF for the American Academy of Sleep Medicine (ed) The AASM manual 2007 for the scoring of sleep and associated events: rules, terminology and technical specifications. American Academy of Sleep Medicine, Westchester, Illinois
O’Connor C, Thornley KS, Hanly PJ (2000) Gender differences in the polysomnographic features of obstructive sleep apnea. Am J Respir Crit Care Med 161:1465–1472
Wahner-Roedler DL, Olson EJ, Narayanan S, Sood R, Hanson AC, Loehrer LL et al (2007) Gender-specific differences in a patient population with obstructive sleep apnea-hypopnea syndrome. Gend Med 4:329–338
Gabbay IE, Lavie P (2012) Age- and gender-related characteristics of obstructive sleep apnea. Sleep Breath 16:453–460
Young T, Evans L, Finn L, Palta M (1997) Estimation of the clinically diagnosed proportion of sleep apnea syndrome in middle-aged men and women. Sleep 20:705–706
Shepertycky MR, Banno K, Kryger MH (2005) Differences between men and women in the clinical presentation of patients diagnosed with obstructive sleep apnea syndrome. Sleep 28:309–314
Quintana-Gallego E, Carmona-Bernal C, Capote F, Sánchez-Armengol A, Botebol-Benhamou G, Polo-Padillo J et al (2004) Gender differences in obstructive sleep apnea syndrome: a clinical study of 1166 patients. Respir Med 98:984–989
Wickwire EM, Collop NA (2010) Insomnia and sleep-related breathing disorders. Chest 137:1449–1463
Luyster FS, Buysse DJ, Strollo PJ Jr (2010) Comorbid insomnia and obstructive sleep apnea: challenges for clinical practice and research. J Clin Sleep Med 6:196–204
Walker RP, Durazo-Arvizu R, Wachter B, Gopalsami C (2001) Preoperative differences between male and female patients with sleep apnea. Laryngoscope 111:1501–1505
Franklin KA, Sahlin C, Stenlund H, Lindberg E (2013) Sleep apnoea is a common occurrence in females. Eur Respir J 41:610–615
Dursunoglu N, Ozkurt S, Sarikaya S (2009) Is the clinical presentation different between men and women admitting to the sleep laboratory? Sleep Breath 13:295–298
Mazzuca E, Battaglia S, Marrone O, Marotta AM, Castrogiovanni A, Esquinas C et al (2014) Gender-specific anthropometric markers of adiposity, metabolic syndrome and visceral adiposity index (VAI) in patients with obstructive sleep apnea. J Sleep Res 23:13–21
Subramanian S, Jayaraman G, Majid H, Aguilar R, Surani S (2012) Influence of gender and anthropometric measures on severity of obstructive sleep apnea. Sleep Breath 16:1091–1095
Newman AB, Foster G, Givelber R, Nieto FJ, Redline S, Young T (2005) Progression and regression of sleep-disordered breathing with changes in weight: the Sleep Heart Health Study. Arch Intern Med 165:2408–2413
Alotair H, Bahammam A (2008) Gender differences in Saudi patients with obstructive sleep apnea. Sleep Breath 12:323–329
Campos-Rodriguez F, Martinez-Garcia MA, de la Cruz-Moron I, Almeida-Gonzalez C, Catalan-Serra P, Montserrat JM (2012) Cardiovascular mortality in women with obstructive sleep apnea with or without continuous positive airway pressure treatment: a cohort study. Ann Intern Med 156:115–122
Subramanian S, Hesselbacher S, Mattewal A, Surani S (2013) Gender and age influence the effects of slow-wave sleep on respiration in patients with obstructive sleep apnea. Sleep Breath 17:51–56
Acknowledgements
The authors thank sleep technicians Bahar Yoruk, Yakup Coskun, and Merve Ozdemir in the Sleep Disorders Laboratory, Department of Chest Diseases, Ege University School of Medicine, for their valuable help in gathering the data related to the health of the patients. The authors also thank Timur Kose from the Department of Biostatistics, Ege University School of Medicine, for statistical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements) or nonfinancial interest (such as personal or professional relationships, affiliations, knowledge, or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study, and no identifying information about participants was available in the article.
Additional information
Comments
This study reports gender associated differences in a cohort of patients with severe OSA. There are many significant differences in clinical presentation and polysomnographic variables between the male and female patients. Women were older, had a higher BMI, increased rate of medical comorbidities and lower AHI; yet, the question is, do these findings accurately characterize OSA in females or are only the most severely affected women referred for polysomnography. It is increasingly recognized that women do not necessarily manifest the characteristic symptoms of OSA. Symptoms not necessarily indicative of OSA but more so insomnia were significantly higher in women than men in this study. Additionally, the increased use of psychotropic medications in women suggests they were treated for a behavioral medicine disorder, insomnia or both. This further suggests women with sleep disturbances refractory to treatment made up a substantial proportion of the female cohort. Current screening questionnaires are likely inadequate in women, which could contribute to delays in diagnosis. Sleep medicine professionals must educate providers to have a heightened clinical suspicion for OSA in women, especially those with insomnia or behavioral medicine disorders that are not responding to treatment.
Vincent Mysliwiec
Tacoma, WA, USA
Rights and permissions
About this article
Cite this article
Basoglu, O.K., Tasbakan, M.S. Gender differences in clinical and polysomnographic features of obstructive sleep apnea: a clinical study of 2827 patients. Sleep Breath 22, 241–249 (2018). https://doi.org/10.1007/s11325-017-1482-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-017-1482-9