Abstract
Background
The objective of the study is to determine the correlations among the variables of dose and the sphincter function (SF) in patients with locally advanced rectal cancer treated with preoperative capecitabine/radiotherapy followed by low anterior resection (LAR) + TME.
Methods
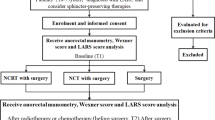
We retrospectively reviewed 92 consecutive patients with LARC treated at our center with LAR from 2006 and more than 2 years free from disease. We re-contoured the anal sphincters (AS) of patients with the help of the radiologist. SF was assessed with the Wexner scale (0–20 points, being punctuation inversely proportional to annal sphincter functionality). All questionnaires were filled out between January 2010 and December 2012. Dosimetric parameters that have been studied include V 20, V 30, V 40, V 50, mean dose (D mean), minimum dose (D min), D 90 (dose received by 90% of the sphincter) and D 98.
Statistical analysis
The correlations among the variables of dose and SF were studied by the Spearman correlation coefficient. Differences in SF relating to maximum doses to the sphincter were assessed by the Mann–Whitney test.
Results
Mean Wexner score was 5.5 points higher in those patients with V 20 > 0 compared to those for which V 20 = 0 (p = 0.008). In a multivariate regression model, results suggest that the effect of V 20 on poor anal sphincter control is independent of the effect of distance, with an adjusted OR of 3.42.
Conclusions
In order to improve the SF in rectal cancer treated with preoperative radiotherapy/capecitabine followed by conservative surgery, the maximum radiation dose to the AS should be limited, when possible, to <20 Gy.


Similar content being viewed by others
References
U.S. Cancer Statistics Working Group. United States Cancer Statistics: 1999–2013 Incidence and Mortality Web-based Report. Atlanta: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention and National Cancer Institute; 2016. http://www.cdc.gov/uscs.
Sauer R, Becker H, Hohenberger W, Rödel C, Wittekind C, Fietkau R, et al. Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med. 2004;351:1731–40.
Wong RKS, Tandan V, De Silva S, Figueredo A. Pre-operative radiotherapy and curative surgery for the management of localized rectal carcinoma. Cochr Datab Syst Rev. 2007, Issue 2. Art. No.: CD002102. doi:10.1002/14651858.CD002102.pub2.
Cedermark B, Johansson H, Rutqvist LE, Wilking N. The Stockholm I Trial of preoperative short term radiotherapy in operable rectal carcinoma. Cancer. 1995;75:2269–75.
Kapiteijn E, Marijnen CA, Nagtegaal ID, Putter H, Steup WH, Wiggers T, et al. Preoperative radiotherapy combined with total mesorectal excision for resectable rectal cancer. N Engl J Med. 2001;345(9):690–2.
Stockholm Colorectal Cancer Study Group & Cedermark. B. Ann Surg Oncol. 1996;3:423.
Folkesson J, Birgisson H, Pahlman L, Cedermark B, Glimelius B. Swedish Rectal Cancer Trial: long lasting benefits from radiotherapy on survival and local recurrence rate. J Clin Oncol. 2005;23:5644–50.
Marijnen CAM, van de Velde CJH, Putter H, van den Brink M, Maas CP, Martijn H, et al. Impact of short-term preoperative radiotherapy on health related quality of life and sexual functioning in primary rectal cancer: report of a multicenter randomized trial. J Clin Oncol. 2005;23:1847–58.
Stephens RJ, Thompson LC, Quirke P, Steele R, Grieve R, Couture J, et al. Impact of short-course preoperative radiotherapy for rectal cancer on patients’ quality of life: data from the Medical Research Council CR07/National Cancer Institute of Canada Clinical Trials Group C016 randomized clinical trial. J Clin Oncol. 2010;28:4233–9.
Yen-TingChen T, Emmertsen KJ, Laurberg S. What are the best questionnaires to capture anorectal function after surgery in rectal cancer? Curr Colorectal Cancer Rep. 2015;11:37–43.
Aaronson NK, Ahmedzai S, Bergman B, Bullinger M, Cull A, et al. The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst. 1993;85:365–76.
Jorge JMN, Wexner SD. Etiology and management of fecal incontinence. Dis Colon Rectum. 1993;36:77–97.
Alsadius D, Hedelin M, Lundstedt D, Pettersson N, Wilderäng U, Steineck G. Mean absorbed dose to the anal-sphincter region and fecal leakage among irradiated prostate cancer survivors. Int J Radiat Oncol Biol Phys. 2012;84:181–5.
Dunberger G, Lind H, Steineck G, Waldenström AC, Nyberg T, Al-Abany M, et al. Self-reported symptoms of faecal incontinence among long-term gynaecological cancer survivors and population-based controls. Eur J Cancer. 2010;46(3):606–15.
Maeda Y, Parés D, Norton C, Vaizey CJ, Kamm MA. Does the St. Mark’s incontinence score reflect patients’ perceptions? A review of 390 patients. Dis Colon Rectum. 2008;51:436–42.
Alburquerque A. Endoanal ultrasonography in fecal incontinence: current and future perspectives. World J Gastrointest Endosc. 2015;7:575–81.
Parangama C, Anu E, Sukria N. Endoanal ultrasound assessment of sphincter defects and thinning—correlation with anal manometry. Arab J Gastroenterol. 2014;15(1):27–31.
Kadoya N. Use of deformable image registration for radiotherapy applications. J Radiol Radiat Ther. 2014;2:1042.
Emmertsen KJ, Laurberg S, Rectal Cancer Function Study Group. Impact of bowel dysfunction on quality of life after sphincter-preserving resection for rectal cancer. Br J Surg. 2013;100(10):1377–87.
Engel J, Kerr J, Schlesinger-Raab A, Eckel R, Sauer H, Hölzel D. Quality of life in rectal cancer patients. A four-year prospective study. Ann Surg. 2003;238(2):203–13.
Schaake W, van der Schaaf A, van Dijk L, Bongaerts A, van den Bergh A, Langendijk J. Normal tissue complication probability (NTCP) models for late rectal bleeding, stool frequency and fecal incontinence after radiotherapy in prostate cancer patients. Radiother and Oncol. 2016;119:381–7.
Acknowledgements
This work has been done thanks to a grant from the “Mutua Madrileña Foundation”. All patients signed the informed consent before entering the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest.
Rights and permissions
About this article
Cite this article
Arias, F., Eito, C., Asín, G. et al. Fecal incontinence and radiation dose on anal sphincter in patients with locally advanced rectal cancer (LARC) treated with preoperative chemoradiotherapy: a retrospective, single-institutional study. Clin Transl Oncol 19, 969–975 (2017). https://doi.org/10.1007/s12094-017-1627-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-017-1627-0