Abstract
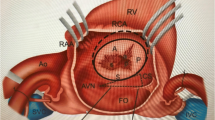
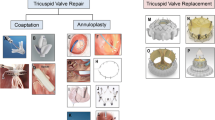
The assessment and management of tricuspid valve disease have evolved substantially during the past several years. Whereas tricuspid stenosis is uncommon, tricuspid regurgitation is frequently encountered and it is most often secondary due to annular dilatation and leaflet tethering from right ventricular remodelling. The indications for tricuspid valve surgery to treat tricuspid regurgitation are several and mainly related to the underlying disease, to the severity of insufficiency and to the right ventricular function. Surgical tricuspid repair has been avoided for years, because of the misleading concept that tricuspid regurgitation should disappear once the primary left-sided problem has been eliminated. Instead, during the last decade, many investigators have reported evidence in favor of a more aggressive surgical approach to functional tricuspid regurgitation, recognising the risk of progressive tricuspid insufficiency in patients with moderate or lesser degrees of tricuspid regurgitation and tricuspid annular dilatation. This concept, along with the long-term outcomes of principal surgical repair techniques are reported and discussed. Last, novel transcatheter therapies have begun to emerge for the treatment of severe tricuspid regurgitation in high-risk patients. Hence, very preliminary pre-clinical and clinical experiences are illustrated. The scope of this review is to explore the anatomic basis, the pathophysiology, the outcomes and the new insights in the management of functional tricuspid regurgitation.


Similar content being viewed by others
References
Cohen SR, Sell JE, McIntosh CL, Clark RE. Tricuspid regurgitation in patients with acquired, chronic, pure mitral regurgitation. I. Prevalence, diagnosis, and comparison of preoperative clinical and hemodynamic features in patients with and without tricuspid regurgitation. J Thorac Cardiovasc Surg. 1987;94:481–7.
Braunwald NS, Ross J, Morrow AG. Conservative management of tricuspid regurgitation in patients undergoing mitral valve replacement. Circulation. 1967;35:I63–9.
Dreyfus GD, Corbi PJ. Chan K M John, Bahrami T: Secondary tricuspid regurgitation or dilatation: which should be the criteria for surgical repair? Ann Thorac Surg. 2005;79:127–32.
Chan V, Burwash IG, Lam B, Auyeung T, Tran A, Mesana TG, Ruel M. Clinical and echocardiographic impact of functional tricuspid regurgitation repair at the time of mitral valve replacement. Ann Thorac Surg. 2009;88:1209–15.
Lee J, Song J, Park JP, Lee JW, Kang D, Song J. Long-term prognosis of isolated significant tricuspid regurgitation. Circ J. 2010;74:375–80.
Fukuda S, Song J, Gillinov AM, McCarthy PM, Daimon M, Kongsaerepong V, Thomas JD, Shiota T. Tricuspid valve tethering predicts residual tricuspid regurgitation after tricuspid annuloplasty. Circulation. 2005;111:975–9.
Onoda K, Yasuda F, Takao M, Shimono T, Tanaka K, Shimpo H, Yada I. Long-term follow-up after Carpentier-Edwards ring annuloplasty for tricuspid regurgitation. Ann Thorac Surg. 2000;70:796–9.
Matsuyama K, Matsumoto M, Sugita T, Nishizawa J, Tokuda Y, Matsuo T, Ueda Y. De Vega annuloplasty and Carpentier-Edwards ring annuloplasty for secondary tricuspid regurgitation. J Heart Valve Dis. 2001;10:520–4.
McCarthy PM, Bhudia SK, Rajeswaran J, Hoercher KJ, Lytle BW, Cosgrove DM, Blackstone EH. Tricuspid valve repair: durability and risk factors for failure. J Thorac Cardiovasc Surg. 2004;127:674–85.
Rivera R, Duran E, Ajuria M. Carpentier’s flexible ring versus De Vega’s annuloplasty. A prospective randomized study. J Thorac Cardiovasc Surg. 1985;89:196–203.
Taramasso M, Vanermen H, Maisano F, Guidotti A, La Canna G, Alfieri O. The growing clinical importance of secondary tricuspid regurgitation. J Am Coll Cardiol. 2012;59:703–10.
Vahanian A, Alfieri O, Andreotti F, Antunes MJ, Barón-Esquivias G, Baumgartner H, Borger MA, Carrel TP, de Bonis M, Evangelista A, Falk V, Iung B, Lancellotti P, Pierard L, Price S, Schäfers H, Schuler G, Stepinska J, Swedberg K, Takkenberg J, Von Oppell UO, Windecker S, Zamorano JL, Zembala M. Guidelines on the management of valvular heart disease (version 2012). Eur Heart J. 2012;33:2451–96.
Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP 3rd, Guyton RA, O’Gara PT, Ruiz CE, Skubas NJ, Sorajja P, Sundt TM 3rd, Thomas JD. 2014 AHA/ACC guideline for the management of patients with valvular heart disease: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2014;63(22):2438–88.
Benedetto U, Melina G, Angeloni E, Refice S, Roscitano A, Comito C, Sinatra R. Prophylactic tricuspid annuloplasty in patients with dilated tricuspid annulus undergoing mitral valve surgery. J Thorac Cardiovasc Surg. 2012;143(3):632–8.
Chikwe J, Itagaki S, Anyanwu A, Adams DH. Impact of concomitant tricuspid annuloplasty on tricuspid regurgitation, right ventricular function, and pulmonary artery hypertension after repair of mitral valve prolapse. J Am Coll Cardiol. 2015;65(18):1931–8.
Goldstone AB, Howard JL, Cohen JE, MacArthur JW Jr, Atluri P, Kirkpatrick JN, Woo YJ. Natural history of coexistent tricuspid regurgitation in patients with degenerative mitral valve disease: implications for future guidelines. J Thorac Cardiovasc Surg. 2014;148(6):2802–9.
Dreyfus GD, Corbi PJ, Chan KM, Bahrami T. Secondary tricuspid regurgitation or dilatation: which should be the criteria for surgical repair? Ann Thorac Surg. 2005;79(1):127–32.
Van de Veire Nico R, Braun J, Delgado V, Versteegh Michel IM, Dion RA, Klautz Robert JM, Bax JJ. Tricuspid annuloplasty prevents right ventricular dilatation and progression of tricuspid regurgitation in patients with tricuspid annular dilatation undergoing mitral valve repair. J Thorac Cardiovasc Surg. 2011;141:1431–9.
Yilmaz O, Suri RM, Dearani JA, Sundt TM 3rd, Daly RC, Burkhart HM, Li Z, Enriquez-Sarano M, Schaff HV. Functional tricuspid regurgitation at the time of mitral valve repair for degenerative leaflet prolapse: the case for a selective approach. J Thorac Cardiovasc Surg. 2011;142(3):608–13.
King RM, Schaff HV, Danielson GK, Gersh BJ, Orszulak TA, Piehler JM, Puga FJ, Pluth JR. Surgery for tricuspid regurgitation late after mitral valve replacement. Circulation. 1984;70:I193–7.
Buzzatti N, Iaci G, Taramasso M, Nisi T, Lapenna E, De Bonis M, Maisano F, Alfieri O. Long-term outcomes of tricuspid valve replacement after previous left-side heart surgery. Eur J Cardiothorac Surg. 2014;46(4):713–9.
Kay JH, Maselli-Campagna G, Tsuji KK. Surgical treatment of tricuspid insufficiency. Ann Surg. 1965;162:53–8.
De Vega NG. La anuloplastia selectiva, regulable y permanente. Una técnica original para el tratamiento de la insuficiencia tricúspide. Rev Esp Cardiol. 1972;25:555–6.
Carpentier A, Deloche A, Hanania G, Forman J, Sellier P, Piwnica A, Dubost C, McGoon DC. Surgical management of acquired tricuspid valve disease. J Thorac Cardiovasc Surg. 1974;67:53–65.
Navia JL, Nowicki ER, Blackstone EH, Brozzi NA, Nento DE, Atik FA, Rajeswaran J, Gillinov AM, Svensson LG, Lytle BW. Surgical management of secondary tricuspid valve regurgitation: annulus, commissure, or leaflet procedure? J Thorac Cardiovasc Surg. 2010;139(1473–1482):e5.
Ghanta RK, Chen R, Narayanasamy N, McGurk S, Lipsitz S, Chen FY, Cohn LH. Suture bicuspidization of the tricuspid valve versus ring annuloplasty for repair of functional tricuspid regurgitation: midterm results of 237 consecutive patients. J Thorac Cardiovasc Surg. 2007;133:117–26.
Nakano S, Kawashima Y, Hirose H, Matsuda H, Shimazaki Y, Taniguchi K, Kawamoto T, Watanabe S, Sakaki S. Evaluation of long-term results of bicuspidalization annuloplasty for functional tricuspid regurgitation. A 17-year experience with 133 consecutive patients. J Thorac Cardiovasc Surg. 1988;95:340–5.
Roshanali F, Saidi B, Mandegar MH, Yousefnia MA, Alaeddini F. Echocardiographic approach to the decision-making process for tricuspid valve repair. J Thorac Cardiovasc Surg. 2010;139:1483–7.
Tang GH, David TE, Singh SK, Maganti MD, Armstrong S, Borger MA. Tricuspid valve repair with an annuloplasty ring results in improved long-term outcomes. Circulation. 2006;114:I577–81.
Nath J, Foster E, Heidenreich PA. Impact of tricuspid regurgitation on long-term survival. J Am Coll Cardiol. 2004;43:405–9.
Katircioglu SF, Yamak B, Ulus AT, Ozsöyler I, Yildiz U, Mavitas B, Birincioglu L, Tasdemir O. Treatment of functional tricuspid regurgitation by bicuspidalization annuloplasty during mitral valve surgery. J Heart Valve Dis. 1997;6:631–5.
Chidambaram M, Abdulali SA, Baliga BG, Ionescu MI. Long-term results of DeVega tricuspid annuloplasty. Ann Thorac Surg. 1987;43:185–8.
Abe T, Tukamoto M, Yanagiya M, Morikawa M, Watanabe N, Komatsu S. De Vega’s annuloplasty for acquired tricuspid disease: early and late results in 110 patients. Ann Thorac Surg. 1989;48:670–6.
Morishita A, Kitamura M, Noji S, Aomi S, Endo M, Koyanagi H. Longterm results after De Vega’s tricuspid annuloplasty. J Cardiovasc Surg (Torino). 2002;43:773–7.
Fukuda S, Gillinov AM, McCarthy PM, Matsumura Y, Thomas JD, Shiota T. Echocardiographic follow-up of tricuspid annuloplasty with a new three-dimensional ring in patients with functional tricuspid regurgitation. J Am Soc Echocardiogr. 2007;20:1236–42.
Dreyfus GD, Raja SG, John KMJ. Tricuspid leaflet augmentation to address severe tethering in functional tricuspid regurgitation. Eur J Cardiothorac Surg. 2008;34:908–10.
Lapenna E, De Bonis M, Verzini A, La Canna G, Ferrara D, Calabrese MC, Taramasso M, Alfieri O. The clover technique for the treatment of complex tricuspid valve insufficiency: midterm clinical and echocardiographic results in 66 patients. Eur J Cardiothorac Surg. 2010;37:1297–303.
Stuge O, Liddicoat J. Emerging opportunities for cardiac surgeons within structural heart disease. J Thorac Cardiovasc Surg. 2006;132:1258–61.
Agarwal S, Tuzcu EM, Rodriguez ER, Tan CD, Rodriguez LL, Kapadia SR. Interventional cardiology perspective of functional tricuspid regurgitation. Circ Cardiovasc Interv. 2009;2:565–73.
Taramasso M, Pozzoli A, Guidotti A, Nietlispach F, Inderbitzin DT, Benussi S, Alfieri O, Maisano F. Percutaneous tricuspid valve therapies: the new frontier. Eur Heart J. 2016. doi:10.1093/eurheartj/ehv766.
Author information
Authors and Affiliations
Corresponding author
Additional information
An erratum to this article can be found at http://dx.doi.org/10.1007/s11748-016-0708-2.
Rights and permissions
About this article
Cite this article
Pozzoli, A., Elisabetta, L., Vicentini, L. et al. Surgical indication for functional tricuspid regurgitation at initial operation: judging from long term outcomes. Gen Thorac Cardiovasc Surg 64, 509–516 (2016). https://doi.org/10.1007/s11748-016-0677-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-016-0677-5