Abstract
Objectives
To evaluate the association between pretreatment MRI descriptors and breast cancer (BC) pathological complete response (pCR) to neoadjuvant chemotherapy (NAC).
Materials and methods
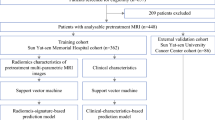
Patients with BC treated by NAC with a breast MRI between 2016 and 2020 were included in this retrospective observational single-center study. MR studies were described using the standardized BI-RADS and breast edema score on T2-weighted MRI. Univariable and multivariable logistic regression analyses were performed to assess variables association with pCR according to residual cancer burden. Random forest classifiers were trained to predict pCR on a random split including 70% of the database and were validated on the remaining cases.
Results
Among 129 BC, 59 (46%) achieved pCR after NAC (luminal (n = 7/37, 19%), triple negative (n = 30/55, 55%), HER2 + (n = 22/37, 59%)). Clinical and biological items associated with pCR were BC subtype (p < 0.001), T stage 0/I/II (p = 0.008), higher Ki67 (p = 0.005), and higher tumor-infiltrating lymphocytes levels (p = 0.016). Univariate analysis showed that the following MRI features, oval or round shape (p = 0.047), unifocality (p = 0.026), non-spiculated margins (p = 0.018), no associated non-mass enhancement (p = 0.024), and a lower MRI size (p = 0.031), were significantly associated with pCR. Unifocality and non-spiculated margins remained independently associated with pCR at multivariable analysis. Adding significant MRI features to clinicobiological variables in random forest classifiers significantly increased sensitivity (0.67 versus 0.62), specificity (0.69 versus 0.67), and precision (0.71 versus 0.67) for pCR prediction.
Conclusion
Non-spiculated margins and unifocality are independently associated with pCR and can increase models performance to predict BC response to NAC.
Clinical relevance statement
A multimodal approach integrating pretreatment MRI features with clinicobiological predictors, including tumor-infiltrating lymphocytes, could be employed to develop machine learning models for identifying patients at risk of non-response. This may enable consideration of alternative therapeutic strategies to optimize treatment outcomes.
Key Points
• Unifocality and non-spiculated margins are independently associated with pCR at multivariable logistic regression analysis.
• Breast edema score is associated with MR tumor size and TIL expression, not only in TN BC as previously reported, but also in luminal BC.
• Adding significant MRI features to clinicobiological variables in machine learning classifiers significantly increased sensitivity, specificity, and precision for pCR prediction.





Similar content being viewed by others
Abbreviations
- BES:
-
Breast Edema Score
- BC:
-
Breast cancer
- BI-RADS:
-
Breast Imaging and Reporting Data System
- HER2:
-
Human epidermal growth factor receptor 2
- NAC:
-
Neoadjuvant chemotherapy
- NME:
-
Non-mass enhancement
- pCR:
-
Pathologic complete response
- RCB:
-
Residual cancer burden
- TIL:
-
Tumor-infiltrating lymphocyte
- TN:
-
Triple negative
References
Wolmark N, Wang J, Mamounas E, Bryant J, Fisher B (2001) Preoperative chemotherapy in patients with operable breast cancer: nine-year results from national surgical adjuvant breast and bowel project b-18. J Natl Cancer Inst Monogr 2001:96–102. https://doi.org/10.1093/oxfordjournals.jncimonographs.a003469
Cortazar P, Zhang L, Untch M et al (2014) Pathological complete response and long-term clinical benefit in breast cancer: the CTNeoBC pooled analysis. Lancet 384:164–172. https://doi.org/10.1016/S0140-6736(13)62422-8
Huober J, Holmes E, Baselga J et al (2019) Survival outcomes of the NeoALTTO study (BIG 1–06): updated results of a randomised multicenter phase III neoadjuvant clinical trial in patients with HER2-positive primary breast cancer. Eur J Cancer 118:169–177. https://doi.org/10.1016/j.ejca.2019.04.038
Spring LM, Fell G, Arfe A et al (2020) Pathologic complete response after neoadjuvant chemotherapy and impact on breast cancer recurrence and survival: a comprehensive meta-analysis. Clin Cancer Res 26:2838–2848. https://doi.org/10.1158/1078-0432.CCR-19-3492
Mann RM, Balleyguier C, Baltzer PA et al (2015) Breast MRI: EUSOBI recommendations for women’s information. Eur Radiol 25:3669–3678. https://doi.org/10.1007/s00330-015-3807-z
Mann RM, Cho N, Moy L (2019) Breast MRI: state of the art. Radiology 292:520–536. https://doi.org/10.1148/radiol.2019182947
Ikeda DM, Hylton NM, Kinkel K et al (2001) Development, standardization, and testing of a lexicon for reporting contrast-enhanced breast magnetic resonance imaging studies. J Magn Reson Imaging 13:889–895. https://doi.org/10.1002/jmri.1127
Uematsu T, Kasami M, Yuen S (2010) Neoadjuvant chemotherapy for breast cancer: correlation between the baseline MR imaging findings and responses to therapy. Eur Radiol 20:2315–2322. https://doi.org/10.1007/s00330-010-1813-8
Eom H-J, Cha JH, Choi WJ, Chae EY, Shin HJ, Kim HH (2017) Predictive clinicopathologic and dynamic contrast-enhanced MRI findings for tumor response to neoadjuvant chemotherapy in triple-negative breast cancer. AJR Am J Roentgenol 208:W225–W230. https://doi.org/10.2214/AJR.16.17125
Bae MS, Shin SU, Ryu HS et al (2016) Pretreatment MR imaging features of triple-negative breast cancer: association with response to neoadjuvant chemotherapy and recurrence-free survival. Radiology 281:392–400. https://doi.org/10.1148/radiol.2016152331
Cheon H, Kim HJ, Kim TH et al (2018) Invasive breast cancer: prognostic value of peritumoral edema identified at preoperative MR imaging. Radiology 287:68–75. https://doi.org/10.1148/radiol.2017171157
Tahmassebi A, Wengert GJ, Helbich TH et al (2019) Impact of machine learning with multiparametric magnetic resonance imaging of the breast for early prediction of response to neoadjuvant chemotherapy and survival outcomes in breast cancer patients. Invest Radiol 54:110–117. https://doi.org/10.1097/RLI.0000000000000518
Liang T, Hu B, Du H, Zhang Y (2020) Predictive value of T2-weighted magnetic resonance imaging for the prognosis of patients with mass-type breast cancer with peritumoral edema. Oncol Lett 20:1–1. https://doi.org/10.3892/ol.2020.12177
Kwon BR, Shin SU, Kim S-Y et al (2022) Microcalcifications and peritumoral edema predict survival outcome in luminal breast cancer treated with neoadjuvant chemotherapy. Radiology 304:310–319. https://doi.org/10.1148/radiol.211509
Kaiser CG, Herold M, Krammer J et al (2017) Prognostic value of “prepectoral edema” in MR-mammography. Anticancer Res 37:1989–1995. https://doi.org/10.21873/anticanres.11542
Uematsu T, Kasami M, Watanabe J (2014) Is evaluation of the presence of prepectoral edema on T2-weighted with fat-suppression 3 T breast MRI a simple and readily available noninvasive technique for estimation of prognosis in patients with breast cancer? Breast Cancer 21:684–692. https://doi.org/10.1007/s12282-013-0440-z
Harada TL, Uematsu T, Nakashima K et al (2021) Evaluation of breast edema findings at T2-weighted breast MRI is useful for diagnosing occult inflammatory breast cancer and can predict prognosis after neoadjuvant chemotherapy. Radiology 299:53–62. https://doi.org/10.1148/radiol.2021202604
Harada TL, Uematsu T, Nakashima K et al (2020) Is the presence of edema and necrosis on T2WI pretreatment breast MRI the key to predict pCR of triple negative breast cancer? Eur Radiol 30:3363–3370. https://doi.org/10.1007/s00330-020-06662-7
Morris EA, Comstock CE, Lee CH (2013) ACR BI-RADS® magnetic resonance imaging. In: ACR BI-RADS® Atlas, Breast Imaging Reporting and Data System. Reston, VA, American College of Radiology
Amin M, Edge S, Greene F et al (2017) AJCC Cancer Staging Manual (8th edition). American Joint Commission on Cancer, Springer International Publishing, Chicago, IL
Elston CW, Ellis IO (1991) Pathological prognostic factors in breast cancer. I. The value of histological grade in breast cancer: experience from a large study with long-term follow-up. Histopathology 19:403–410. https://doi.org/10.1111/j.1365-2559.1991.tb00229.x
Salgado R, Denkert C, Demaria S et al (2015) The evaluation of tumor-infiltrating lymphocytes (TILs) in breast cancer: recommendations by an International TILs Working Group 2014. Ann Oncol 26:259–271. https://doi.org/10.1093/annonc/mdu450
Kim KI, Lee KH, Kim TR, Chun YS, Lee TH, Park HK (2014) Ki-67 as a predictor of response to neoadjuvant chemotherapy in breast cancer patients. J Breast Cancer 17:40–46. https://doi.org/10.4048/jbc.2014.17.1.40
Russo L, Maltese A, Betancourt L et al (2019) Locally advanced breast cancer: tumor-infiltrating lymphocytes as a predictive factor of response to neoadjuvant chemotherapy. Eur J Surg 45:963–968. https://doi.org/10.1016/j.ejso.2019.01.222
Petrelli F, Viale G, Cabiddu M, Barni S (2015) Prognostic value of different cut-off levels of Ki-67 in breast cancer: a systematic review and meta-analysis of 64,196 patients. Breast Cancer Res Treat 153:477–491. https://doi.org/10.1007/s10549-015-3559-0
Wolff AC, Hammond MEH, Allison KH et al (2018) Human epidermal growth factor receptor 2 testing in breast cancer: american society of clinical oncology/college of american pathologists clinical practice guideline focused update. J Clin Oncol 36:2105–2122. https://doi.org/10.1200/JCO.2018.77.8738
Symmans WF, Peintinger F, Hatzis C et al (2007) Measurement of residual breast cancer burden to predict survival after neoadjuvant chemotherapy. J Clin Oncol 25:4414–4422. https://doi.org/10.1200/JCO.2007.10.6823
Goorts B, van Nijnatten TJA, de Munck L et al (2017) Clinical tumor stage is the most important predictor of pathological complete response rate after neoadjuvant chemotherapy in breast cancer patients. Breast Cancer Res Treat 163:83–91. https://doi.org/10.1007/s10549-017-4155-2
Livingston-Rosanoff D, Schumacher J, Walle KV et al (2019) Does tumor size predict response to neoadjuvant chemotherapy in the modern era of biologically driven treatment? A nationwide study of US breast cancer patients. Clin Breast Cancer 19:e741–e747. https://doi.org/10.1016/j.clbc.2019.05.014
Baron P, Beitsch P, Boselli D et al (2016) Impact of tumor size on probability of pathologic complete response after neoadjuvant chemotherapy. Ann Surg Oncol 23:1522–1529. https://doi.org/10.1245/s10434-015-5030-1
Korde LA, Somerfield MR, Carey LA et al (2021) Neoadjuvant chemotherapy, endocrine therapy, and targeted therapy for breast cancer: asco guideline. J Clin Oncol 39:1485–1505. https://doi.org/10.1200/JCO.20.03399
Kim S-Y, Cho N, Choi Y et al (2021) Factors affecting pathologic complete response following neoadjuvant chemotherapy in breast cancer: development and validation of a predictive nomogram. Radiology 299:290–300. https://doi.org/10.1148/radiol.2021203871
Wein L, Savas P, Luen SJ, Virassamy B, Salgado R, Loi S (2017) Clinical validity and utility of tumor-infiltrating lymphocytes in routine clinical practice for breast cancer patients: current and future directions. Front Oncol. https://doi.org/10.3389/fonc.2017.00156
Braman N, Prasanna P, Whitney J et al (2019) Association of peritumoral radiomics with tumor biology and pathologic response to preoperative targeted therapy for HER2 (erbb2)-positive breast cancer. JAMA Netw Open 2:e192561. https://doi.org/10.1001/jamanetworkopen.2019.2561
Wu J, Li X, Teng X et al (2018) Magnetic resonance imaging and molecular features associated with tumor-infiltrating lymphocytes in breast cancer. Breast Cancer Res 20:101. https://doi.org/10.1186/s13058-018-1039-2
Lee H, Lee JE, Jeong WG et al (2022) Her2-positive breast cancer: association of mri and clinicopathologic features with tumor-infiltrating lymphocytes. AJR Am J Roentgenol 218:258–269. https://doi.org/10.2214/AJR.21.26400
Shin SU, Cho N, Lee H-B et al (2018) Neoadjuvant chemotherapy and surgery for breast cancer: preoperative MRI features associated with local recurrence. Radiology 289:30–38. https://doi.org/10.1148/radiol.2018172888
Symmans WF, Peintinger F, Hatzis C et al (2007) Measurement of residual breast cancer burden to predict survival after neoadjuvant chemotherapy. J Clin Oncol 25:4414–4422. https://doi.org/10.1200/JCO.2007.10.6823
Hamy A-S, Darrigues L, Laas E et al (2020) Prognostic value of the residual cancer burden index according to breast cancer subtype: validation on a cohort of bc patients treated by neoadjuvant chemotherapy. PLoS One 15:e0234191. https://doi.org/10.1371/journal.pone.0234191
Çelebi F, Agacayak F, Ozturk A et al (2020) Usefulness of imaging findings in predicting tumor-infiltrating lymphocytes in patients with breast cancer. Eur Radiol 30:2049–2057. https://doi.org/10.1007/s00330-019-06516-x
Ku YJ, Kim HH, Cha JH et al (2016) Correlation between MRI and the level of tumor-infiltrating lymphocytes in patients with triple-negative breast cancer. AJR Am J Roentgenol 207:1146–1151. https://doi.org/10.2214/AJR.16.16248
Hamy A-S, Bonsang-Kitzis H, Croze DD et al (2019) Interaction between molecular subtypes and stromal immune infiltration before and after treatment in breast cancer patients treated with neoadjuvant chemotherapy. Clin Cancer Res 25:6731–6741. https://doi.org/10.1158/1078-0432.CCR-18-3017
Chamming’s F, Ueno Y, Ferré R et al (2018) Features from computerized texture analysis of breast cancers at pretreatment mr imaging are associated with response to neoadjuvant chemotherapy. Radiology 286:412–420. https://doi.org/10.1148/radiol.2017170143
Saint Martin M-J, Orlhac F, Akl P et al (2021) A radiomics pipeline dedicated to Breast MRI: validation on a multi-scanner phantom study. MAGMA 34:355–366. https://doi.org/10.1007/s10334-020-00892-y
Granzier RWY, van Nijnatten TJA, Woodruff HC, Smidt ML, Lobbes MBI (2019) Exploring breast cancer response prediction to neoadjuvant systemic therapy using MRI-based radiomics: a systematic review. Eur J Radiol 121:108736. https://doi.org/10.1016/j.ejrad.2019.108736
Pepe MS, Kerr KF, Longton G, Wang Z (2013) Testing for improvement in prediction model performance. Stat Med 32:1467–1482. https://doi.org/10.1002/sim.5727
Acknowledgements
We thank Laetitia Chanas, Maud Milder, Mathieu Carton and Alexia Savignoni for their assistance with the compilation of the data.
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Caroline Malhaire.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors has significant statistical expertise (Caroline Malhaire).
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• observational
• performed at one institution
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Malhaire, C., Selhane, F., Saint-Martin, MJ. et al. Exploring the added value of pretherapeutic MR descriptors in predicting breast cancer pathologic complete response to neoadjuvant chemotherapy. Eur Radiol 33, 8142–8154 (2023). https://doi.org/10.1007/s00330-023-09797-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-09797-5