Abstract
Background
Poor COVID-19 outcomes occur with higher frequency in people with rheumatic and musculoskeletal diseases (RMD). Better understanding of the factors involved is crucial to informing patients and clinicians regarding risk mitigation.
Aim
To describe COVID-19 outcomes for people with RMD in Ireland over the first 2 years of the pandemic.
Methods
Data entered into the C19-GRA provider registry from Ireland between 24th March 2020 and 31st March 2022 were analysed. Differences in the likelihood of hospitalisation and mortality according to demographic and clinical variables were investigated.
Results
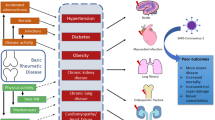
Of 237 cases included, 59.9% were female, 95 (41.3%) were hospitalised, and 22 (9.3%) died. Hospitalisation was more common with increasing age, gout, smoking, long-term glucocorticoid use, comorbidities, and specific comorbidities of cardiovascular and pulmonary disease, and cancer. Hospitalisation was less frequent in people with inflammatory arthritis and conventional synthetic or biologic disease-modifying antirheumatic drug use. Hospitalisation had a U-shaped relationship with disease activity, being more common in both high disease activity and remission. Mortality was more common with increasing age, gout, smoking, long-term glucocorticoid use, comorbidities, and specific comorbidities of cardiovascular disease, pulmonary disease, and obesity. Inflammatory arthritis was less frequent in those who died.
Conclusion
Hospitalisation or death were more frequently experienced by RMD patients with increasing age, certain comorbidities including potentially modifiable ones, and certain medications and diagnoses amongst other factors. These are important ‘indicators’ that can help risk-stratify and inform the management of RMD patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and consequent Coronavirus disease 2019 (COVID-19) is an ongoing global health challenge. People with rheumatic and musculoskeletal disease (RMD) who develop COVID-19 may have worse prognosis compared to the general population [1]. The improvements in outcomes of COVID-19 that have occurred in the general population over time may not be seen in the RMD population [2,3,4]. Vaccination against SARS-CoV-2 offers protection in people with RMD; however, immunomodulating medications may prevent optimal vaccine responses in a small number of patients [5].
As public health restrictions lessen and increased interpersonal interactions occur in work and social settings, it becomes of increased importance to report data that people with RMD can use to understand the potential health implications. Exploration of the outcomes of COVID-19 in people with RMD and the associations with disease and individual specific factors may facilitate more precise/accurate risk assessments.
In this study, we report COVID-19 outcomes in people with RMD in Ireland over the first 2 years of the pandemic.
Methods
COVID-19 Global Rheumatology Alliance
Data regarding individuals with RMD with COVID-19 are entered into one of two parallel international data portals hosted in the USA and UK. Details of the C19-GRA registries have been published previously [6, 7].
Data collection
Data input into the C19-GRA provider registry took place between 24th March 2020 and 31st March 2022 and included baseline RMD status including demographic and clinical variables such as age, sex, smoking status, RMD diagnosis, disease activity (as per the physician's global assessment (remission, low, moderate, or high/severe)), and comorbidities. All diagnoses were physician-reported. Medications were categorised as previously described [8]. Disease-modifying antirheumatic drugs (DMARDs) were grouped as conventional synthetic DMARDs (csDMARDs) or biologic DMARDs (bDMARDs) and targeted synthetic DMARDs (tsDMARDs) [6]. RMDs were categorised as (1) inflammatory arthritis (IA) (rheumatoid arthritis, psoriatic arthritis, spondyloarthritis, juvenile idiopathic arthritis); (2) gout; (3) vasculitis, connective tissue diseases, and all other diagnoses (‘other’). Data collected regarding COVID-19 infection included method of diagnosis, place of diagnosis, COVID-19 symptoms, and outcomes of COVID-19 disease including hospitalisation, ventilation, and death.
Demographic and clinical continuous variables were reported as median (Interquartile range (IQR)) and categorical variables as number and percentage (%). Hospitalisation and mortality probability were calculated for each category of the key demographic and clinical variables. Differences in the likelihood of hospitalisation and mortality according to demographic and clinical variables were investigated using Chi-squared test or Fisher’s exact test, as appropriate.
All statistical analyses were performed and graphs were prepared using STATA IC15 (StataCorp. 2017. Stata Statistical Software: Release 15. College Station, TX: StataCorp LLC.).
This study was approved by the Irish National Research Ethics Committee for COVID-19 (20-NREC-COV-010). The committee waived the need for written informed consent as the data were anonymised.
Results
Over the 2-year period, 237 cases of COVID-19 were reported in people with RMD (Table 1). The majority (59.9%) were female. Inflammatory arthritis (IA) was the most common diagnostic grouping (154/237, 65%), with the remainder having gout (35/237, 14.8%) and CTD/vasculitis/others (57/237, 24.1%). Most patients (46.5%) were in remission, 36.5% had low disease activity, 14.8% moderate disease activity, and 2.2% high disease activity. Eighty cases (33.8%) had no comorbidities. The most frequent comorbidities were cardiovascular disease (40.5%), pulmonary disease (16.9%), and obesity (9.7%). Of the 237 cases, 95 (41.3%) were hospitalised and 22 (9.3%) died.
Hospitalisation outcome
Demographic and clinical details according to hospitalisation are shown in Table 1. Hospitalisation was more frequently experienced with increasing age, a diagnosis of gout, smoking, long-term glucocorticoid use, comorbidities, and specific comorbidities of cardiovascular and pulmonary disease, and cancer. A diagnosis of inflammatory arthritis and conventional synthetic or biologic disease-modifying antirheumatic drug use were less common in those hospitalised. Hospitalisation appeared to have a U-shaped relationship with disease activity, being more common both in patients with high disease activity and those in remission (Fig. 1).
Mortality outcome
Demographic and clinical details according to mortality are shown in Table 1. Mortality was more common with increasing age, a diagnosis of gout, smoking, long-term glucocorticoid use, comorbidities, and specific comorbidities of cardiovascular disease, pulmonary disease, and obesity. A diagnosis of inflammatory arthritis was less common in those who died.
Discussion
This is the largest and most comprehensive study of outcomes of people with RMD and COVID-19 from Ireland. As reported in the general population, we found increasing age, comorbidities, specific comorbidities of cardiovascular and pulmonary disease, and obesity, and smoking to be positively associated with severe outcomes of hospitalisation or death. We have also identified potential RMD specific associations, with long-term glucocorticoid use and a diagnosis of gout more common, and a diagnosis of inflammatory arthritis, and conventional synthetic or biologic disease-modifying antirheumatic drug use less frequent in those with severe outcomes. RMD activity appeared to have a biphasic effect, with severe outcomes being more common in those with high disease activity and those with remission; this may be modulated by diagnostic group, particularly with gout patients (who otherwise had worse outcomes) being more likely to have disease activity labelled as “remission” between gout flares. However, the U-shaped relationship remained following exclusion of patients with gout.
The RMD-specific factors we have identified as being more frequent among RMD patients in Ireland with poor outcomes are broadly in keeping with previous studies in this area. Glucocorticoid use prior to the development of COVID-19, particularly in doses ≥ 10 mg/day have been associated with COVID-19-related hospitalisation and mortality [6, 9]. Increasing disease activity and its synergistic effect with increasing glucocorticoid doses has also been associated with more severe outcomes [9, 10]. Whether certain RMD groups or specific diagnoses within groupings are associated with worse outcomes is more difficult to ascertain with different studies reporting disparate findings [9, 11, 12]. Studies have demonstrated that specific medications such as rituximab, cyclophosphamide, and mycophenolate mofetil appear to be associated with more severe outcomes [9, 13, 14]. The potential for improved outcomes with individual medications or medication groups such as csDMARDs and bDMARDs is more controversial [8, 15].
Our study has several limitations. While this is the largest study of people with RMD and COVID-19 from Ireland, the statistical power of our study is limited by the relatively low number of cases reported, prohibiting the undertaking of multivariable analyses. The findings of our study must be interpreted with due cognisance of the limitations of the C19-GRA registry, including selection bias, unmeasured confounders, and possible artefact related to the identification of milder cases over time as testing capacity expanded [16]. The C19-GRA is a physician-entered registry and is limited by selection bias with a likely tendency to report more severe cases. It is also a case-based registry with no denominator population; therefore, inferences cannot be drawn about the incidence of COVID-19 in people with RMDs. Additionally, the C19-GRA is by design restricted to people with RMD and COVID-19; therefore, comparisons cannot be made to people with non-RMD and COVID-19 nor to RMD in the absence of COVID-19. We have reported data previously from the TRACR study which utilised a rigorous case ascertainment methodology; these results are broadly in keeping with the overall results reported here and should ameliorate some of the concerns regarding potential selection bias [4, 17]. The COVID-19 vaccination programme in Ireland occurred in parallel with the collection of data in this study and may have impacted findings; however, we have previously demonstrated no change in outcomes over time [4].
In conclusion, we have identified both shared features with the general population and RMD-specific factors which are over-represented among patients with severe COVID-19 outcomes. These factors may aid early identification of patients with RMDs with poor prognosis when prioritising booster vaccination and when prescribing COVID-19 antiviral therapy.
Data availability
The data underlying this article are available on reasonable request to the corresponding author.
Data sharing statement
Request for access to data from the registry should be made to the Data Access and Sharing Committee of the COVID-19 Global Rheumatology Alliance.
References
Conway R, Grimshaw AA, Konig MF et al (2022) SARS-CoV-2 Infection and COVID-19 Outcomes in rheumatic diseases: a systematic literature review and meta-analysis. Arthritis Rheumatol (Hoboken, NJ) 74(5):766–775
Anesi GL, Jablonski J, Harhay MO et al (2021) Characteristics, outcomes, and trends of patients with COVID-19-related critical illness at a learning health system in the United States. Ann Intern Med 174(5):613–621
Roth GA, Emmons-Bell S, Alger HM et al (2021) Trends in patient characteristics and COVID-19 in-hospital mortality in the United States during the COVID-19 pandemic. JAMA Netw Open 4(5):e218828–e
Conway R, Nikiphorou E, Demetriou CA et al (2022) Temporal trends in COVID-19 outcomes in people with rheumatic diseases in Ireland: data from the COVID-19 Global Rheumatology Alliance registry. Rheumatol (Oxford) 61(SI2):SI151–SI6
Wieske L, van Dam KPJ, Steenhuis M et al (2022) Humoral responses after second and third SARS-CoV-2 vaccination in patients with immune-mediated inflammatory disorders on immunosuppressants: a cohort study. Lancet Rheumatol 4(5):e338–e350
Gianfrancesco M, Hyrich KL, Al-Adely S et al (2020) Characteristics associated with hospitalisation for COVID-19 in people with rheumatic disease: data from the COVID-19 Global Rheumatology Alliance physician-reported registry. Ann Rheum Dis 79(7):859–866
Gianfrancesco MA, Hyrich KL, Gossec L et al (2020) Rheumatic disease and COVID-19: initial data from the COVID-19 Global Rheumatology Alliance provider registries. Lancet Rheumatol 2(5):e250–e253
Conway R, Nikiphorou E, Demetriou CA et al (2021) Predictors of hospitalization in patients with rheumatic disease and COVID-19 in Ireland: data from the COVID-19 global rheumatology alliance registry. Rheumatol Adv Pract 5(2)
Strangfeld A, Schafer M, Gianfrancesco MA et al (2021) Factors associated with COVID-19-related death in people with rheumatic diseases: results from the COVID-19 Global Rheumatology Alliance physician-reported registry. Ann Rheum Dis 80(7):930–942
Schäfer M, Strangfeld A, Hyrich KL et al (2021) Response to: ‘Correspondence on ‘Factors associated with COVID-19-related death in people with rheumatic diseases: results from the COVID-19 Global Rheumatology Alliance physician reported registry’’ by Mulhearn et al. Ann Rheum Dis annrheumdis-2021–220134
Pablos JL, Galindo M, Carmona L et al (2020) Clinical outcomes of hospitalised patients with COVID-19 and chronic inflammatory and autoimmune rheumatic diseases: a multicentric matched cohort study. Ann Rheum Dis 79(12):1544–1549
Sattui SE, Conway R, Putman MS et al (2021) Outcomes of COVID-19 in patients with primary systemic vasculitis or polymyalgia rheumatica from the COVID-19 Global Rheumatology Alliance physician registry: a retrospective cohort study. Lancet Rheumatol 3(12):e855–e864
Sparks JA, Wallace ZS, Seet AM et al (2021) Associations of baseline use of biologic or targeted synthetic DMARDs with COVID-19 severity in rheumatoid arthritis: results from the COVID-19 Global Rheumatology Alliance physician registry. Ann Rheum Dis 80(9):1137–1146
Felten R, Duret PM, Bauer E et al (2022) B-cell targeted therapy is associated with severe COVID-19 among patients with inflammatory arthritides: a 1-year multicentre study in 1116 successive patients receiving intravenous biologics. Ann Rheum Dis 81(1):143–145
Izadi Z, Brenner EJ, Mahil SK et al (2021) Association between tumor necrosis factor inhibitors and the risk of hospitalization or death among patients with immune-mediated inflammatory disease and COVID-19. JAMA Netw Open 4(10):e2129639
Gianfrancesco MA, Robinson PC (2021) Changing COVID-19 outcomes in patients with rheumatic disease-are we really getting better at this? Lancet Rheumatol 3(2):e88–e90
Flood RM, Conway R, Kirby C et al (2020) Correspondence to: 'Characteristics associated with hospitalisation for COVID-19 in people with rheumatic disease: data from the COVID-19 Global Rheumatology Alliance physician-reported registry' by Gianfrancesco et al. Ann Rheum Dis annrheumdis 218733
Acknowledgements
The authors would like to thank all rheumatology providers who entered data into the registry.
Funding
Open Access funding provided by the IReL Consortium.
Author information
Authors and Affiliations
Consortia
Contributions
RC, CL, KL, JGR, RK, ADF, JJC, POC, RMF, RHM, DJK, NA, FS, and GMM contributed to data collection, data quality control, data analysis, and interpretation. They drafted, and revised, the manuscript critically for important intellectual content and gave final approval of the version to be published. EN and CAD contributed to the analysis and interpretation of the data. They drafted, and revised, the manuscript critically for important intellectual content and gave final approval of the version to be published. PCR, JWL, and RG directed the work and contributed to the analysis and interpretation of the data. They drafted, and revised, the manuscript critically for important intellectual content and gave final approval of the version to be published.
Corresponding author
Ethics declarations
The views expressed here are those of the authors and do not necessarily represent the views of the American College of Rheumatology (ACR), the European Alliance of Associations for Rheumatology (EULAR), and the (UK) National Health Service (NHS), the National Institute for Health Research (NIHR) or the (UK) Department of Health.
Ethics approval
Irish National Research Ethics Committee for COVID-19 (20-NREC-COV-010).
Conflict of interest
Richard Conway: speakers bureau Janssen, Roche, Sanofi, Abbvie, Clinical Trials: Abbvie, grant/research support: Janssen; Elena Nikiphorou: speakers bureau: AbbVie, Eli-Lilly, Gilead, Celltrion, Pfizer, Sanofi, Fresenius, grant/research support: Pfizer, Lilly; Christiana Demetriou: none declared; Candice Low: none declared; Kelly Leamy: none declared; John Ryan: none declared; Ronan Kavanagh: none declared; Alexander Fraser: none declared; John Carey: none declared; Paul O'Connell: none declared; Rachael Flood: none declared; Ronan Mullan: none declared; David Kane: none declared; Nicola Ambrose: none declared; Frances Stafford: none declared; Philip Robinson speakers bureau: UCB, Roche, Pfizer, Gilead, Janssen, Novartis; Eli Lilly, Abbvie, grant/research support from: Abbvie, UCB, Novartis, Janssen, Pfizer; Jean Liew: grant/research support from: Pfizer. Rebecca Grainger: speakers bureau: Pfizer, Cornerstones, Janssen, Novartis; Abbvie; Geraldine McCarthy: none declared.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Conway, R., Nikiphorou, E., Demetriou, C.A. et al. Outcomes of COVID-19 in people with rheumatic and musculoskeletal disease in Ireland over the first 2 years of the pandemic. Ir J Med Sci 192, 2495–2500 (2023). https://doi.org/10.1007/s11845-022-03265-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-022-03265-7