Abstract
Purpose
To assess the outcome of surgically fixated femur shaft and distal femur fractures following low-velocity civilian gunshot injuries over a 4-year period.
Methods
A retrospective review was conducted on all patients who sustained femur shaft and distal femur fractures from civilian low-velocity gunshot injuries that required definitive surgical fixation between January 2014 and December 2017. Patient demographics, comorbidities, injury characteristics, duration between injury and surgical fixation and presence of complications were captured.
Results
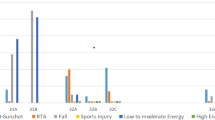
A total of 122 patients (mean age, 29.1 ± 9.5 years) were included. Supracondylar femur fractures (AO 33) accounted for 49% of total injuries, followed by femoral shaft (AO 32) and intra-articular distal femur fractures (AO 33 B & C) with 40% and 11%, respectively. Intramedullary nail fixation was the choice of treatment for femur shaft fractures (49.98%) and supracondylar fractures (63%). Intra-articular injuries were predominantly treated with distal femoral locking plates (85%). Arterial and nerve injuries were the most commonly encountered associated injuries occurring in five patients (4.1%) each. Fracture-related infection was diagnosed in two patients (1.6%). No cases of non-union and compartment syndrome were recorded.
Conclusion
Femur shaft and supracondylar fractures fixated with intramedullary nails are associated with low complication rates and perfect union rates. Our study suggests that intra-articular distal femur fractures fixated with locking plates and cannulated screws have a high complication rate and poorer surgical outcomes. Non-union and compartment syndrome are rare complications of gunshot femur fractures fixated with either intramedullary nails or locking plates.


Similar content being viewed by others
Availability of data and materials
Due to the protection of personal information act of the country of origin, raw data cannot be made available without formal ethics approval. Any requests for future collaboration should be submitted to the authors.
References
UNODC (2019) Global Study on Homicide 2019. In: Vienna. https://www.unodc.org/documents/data-and-analysis/gsh/Booklet1.pdf. Accessed 4 Jul 2021
Thomson J. A MURDEROUS LEGACY: coloured homicide trends in South Africa. S Af Crime Q. 2016. https://doi.org/10.17159/2413-3108/2004/v0i7a1050.
Martin C, Thiart G, McCollum G, et al. The burden of gunshot injuries on orthopaedic healthcare resources in south Africa. S Afr Med J. 2017;107:626–30. https://doi.org/10.7196/SAMJ.2017.v107i7.12257.
Abghari M, Monroy A, Schubl S, Davidovitch R, Egol K. Outcomes following low-energy civilian gunshot wound trauma to the lower extremities: results of a standard protocol at an urban trauma Center. Iowa Orthop J 2015;35:65–9.
Nowotarski P, Brumback RJ. Immediate interlocking nailing of fractures of the femur caused by low-to mid-velocity gunshots. J Orthop Trauma. 1994. https://doi.org/10.1097/00005131-199404000-00010.
Ryan JR, Hensel RT, Salciccioli GG, Pedersen HE. Fractures of the femur secondary to low-velocity gunshot wounds. J Trauma Inj Infect Crit Care. 1981. https://doi.org/10.1097/00005373-198102000-00012.
Bergman M, Tornetta P, Kerina M, et al. Femur fractures caused by gunshots: Treatment by immediate reamed intramedullary nailing. J Trauma - Inj Infect Crit Care. 1993. https://doi.org/10.1097/00005373-199306000-00005.
Nicholas RM, McCoy GF. Immediate intramedullary nailing of femoral shaft fractures due to gunshots. Injury. 1995. https://doi.org/10.1016/0020-1383(95)00012-X.
Levy AS, Wetzler MJ, Guttman G, Covall DJ, Fink B, Whitelaw GP, Kozin S. Treating gunshot femoral shaft fractures with immediate reamed intramedullary nailing. Orthop Rev 1993;22(7):805–9.
Winquist RA, Hansen ST, Clawson DK. Closed intramedullary nailing of femoral fractures. A report of five hundred and twenty cases. J Bone Jt Surg Ser A. 1984. https://doi.org/10.2106/00004623-198466040-00006.
Brien WW, Kuschner SH, Brien EW, Wiss DA. The management of gunshot wounds to the femur. Orthop Clin N Am 1995;26(1):133–8.
Wiss DA, Brien WW, Becker V. Interlocking nailing for the treatment of femoral fractures due to gunshot wounds. J Bone Jt Surg Ser A. 1991. https://doi.org/10.2106/00004623-199173040-00018.
Dougherty PJ, Gherebeh P, Zekaj M, et al. Retrograde versus antegrade intramedullary nailing of gunshot diaphyseal femur fractures. Clin Orthop Relat Res. 2013;471(12):3974–80.
Cannada LK, Jones TR, Guerrero-Bejarano M, et al. Retrograde intramedullary nailing of femoral diaphyseal fractures caused by low-velocity gunshots. Orthopedics. 2009. https://doi.org/10.3928/01477447-20090301-05.
Poyanli O, Unay K, Akan K, et al. No evidence of infection after retrograde nailing of supracondylar femur fracture in gunshot wounds. J Trauma Inj Infect Crit Care. 2010;68:970–4. https://doi.org/10.1097/TA.0b013e3181bb974b.
Gangavalli AK, Nwachuku CO. Management of distal femur fractures in adults. an overview of options. Orthop Clin North Am. 2016;47:85–96.
Meinberg EG, Agel J, Roberts CS, et al. Fracture and dislocation classification compendium-2018. J Orthop Trauma. 2018. https://doi.org/10.1097/BOT.0000000000001063.
Metsemakers WJ, Kuehl R, Moriarty TF, et al. Infection after fracture fixation: Current surgical and microbiological concepts. Injury. 2018;49:511–22.
Litrenta J, Tornetta P, Mehta S, et al. Determination of radiographic healing: an assessment of consistency using RUST and modified RUST in metadiaphyseal fractures. J Orthop Trauma. 2015;29:516–20. https://doi.org/10.1097/BOT.0000000000000390.
Nandra R, Grover L, Porter K. Fracture non-union epidemiology and treatment. Trauma. 2016;18:3–11.
Sofianos C (2021) Under the power of the gun—the Mail & Guardian. In: Mail Guard. https://mg.co.za/news/2021-01-10-under-the-power-of-the-gun/. Accessed 4 Jul 2021
Davies R (2019) Army deployed as gang violence escalates to unprecedent. In: Dly. Maverick. https://www.dailymaverick.co.za/article/2019-07-12-army-deployed-as-gang-violence-escalates-to-unprecedented-levels-and-residents-cry-out-for-help/. Accessed 4 Jul 2021
Jakoet MS, Burger M, Van Heukelum M, et al. The epidemiology and orthopaedic burden of civilian gunshot injuries over a four-year period at a level one trauma unit in Cape Town, South Africa. Int Orthop. 2020. https://doi.org/10.1007/s00264-020-04723-6.
van Heukelum M, le Roux N, Jakoet S, Ferreira N. Financial burden of orthopaedic gunshot-related injury management at a major trauma centre. S Afr Med J. 2020;110:882–6. https://doi.org/10.7196/SAMJ.2020.v110i9.14638.
Ali MA, Hussain SA, Khan MS. Evaluation of results of interlocking nails in femur fractures due to high velocity gunshot injuries. J Ayub Med Coll Abbottabad 2008;20(1):16–9.
Woolum JA, Bailey AM, Dugan A, et al. Evaluation of infection rates with narrow versus broad-spectrum antibiotic regimens in civilian gunshot open-fracture injury. Am J Emerg Med. 2020;38:934–9. https://doi.org/10.1016/j.ajem.2019.158358.
Papasoulis E, Patzakis MJ, Zalavras CG. Antibiotics in the treatment of low-velocity gunshot-induced fractures: a systematic literature review trauma. Clin Orthop Relat Res. 2013;471:3937–44.
Polat G, Balci HI, Ergin ON, et al. A comparison of external fixation and locked intramedullary nailing in the treatment of femoral diaphysis fractures from gunshot injuries. Eur J Trauma Emerg Surg. 2018. https://doi.org/10.1007/s00068-017-0814-6.
Meccariello L, Bisaccia M, Ronga M, et al. Locking retrograde nail, non-locking retrograde nail and plate fixation in the treatment of distal third femoral shaft fractures: radiographic, bone densitometry and clinical outcomes. J Orthop Traumatol. 2021. https://doi.org/10.1186/s10195-021-00593-9.
Dorlac WC, DeBakey ME, Holcomb JB, et al. Mortality from isolated civilian penetrating extremity injury. J Trauma Inj Infect Crit Care. 2005;59:217–22.
Moed BR, Fakhouri AJ. Compartment syndrome after low-velocity gunshot wounds to the forearm. J Orthop Trauma. 1991. https://doi.org/10.1097/00005131-199105020-00003.
Mehta SK, Dale WW, Dedwylder MD, et al. Rates of neurovascular injury, compartment syndrome, and early infection in operatively treated civilian ballistic forearm fractures. Injury. 2018. https://doi.org/10.1016/j.injury.2018.10.009.
Knab LM, Abuzeid A, Rodriguez H, Issa N. Thigh compartment syndrome in urban trauma: bullets to blame, not collisions. J Surg Res. 2013. https://doi.org/10.1016/j.jss.2013.07.003.
Holbein O, Strecker W, Rath SA, Kinzl L. Compartment syndrome of the thigh with sciatic nerve palsy. J Orthop Trauma. 2000. https://doi.org/10.1097/00005131-200008000-00018.
Kiran Kumar GN, Sharma G, Farooque K, et al. Locking compression plate in distal femoral intra-articular fractures: our experience. Int Sch Res Not. 2014. https://doi.org/10.1155/2014/372916.
McQuirter JL, Rothenberg SJ, Dinkins GA, et al. Change in blood lead concentration up to 1 year after a gunshot wound with a retained bullet. Am J Epidemiol. 2004;159:683–92. https://doi.org/10.1093/aje/kwh074.
Riehl JT, Connolly K, Haidukewych G, Koval K. Fractures due to gunshot wounds: do retained bullet fragments affect union? Iowa Orthop J. 2015;35:55–61.
Johnson DJ, Versteeg GH, Middleton JA, et al. Epidemiology and risk factors for loss to follow-up following operatively treated femur ballistic fractures. Injury. 2021. https://doi.org/10.1016/j.injury.2021.06.012.
Acknowledgements
The authors would like to thank two anonymous reviewers for their comments and suggestions in order to improve this manuscript.
Funding
No funding has been received for this manuscript.
Author information
Authors and Affiliations
Contributions
The authors confirm that all authors have made substantial contributions to all of the following: The conception and design of the study, or acquisition of data, or analysis and interpretation of data. Drafting the article or revising it critically for important intellectual content. Final approval of the version to be submitted. Sound scientific research practice. The authors further confirm that: The manuscript, including related data, figures and tables has not been previously published and is not under consideration elsewhere. No data have been fabricated or manipulated (including images) to support your conclusions. This submission does not represent a part of single study that has been split up into several parts to increase the quantity of submissions and submitted to various journals or to one journal over time (e.g. “salami-publishing”). OM contributed to study conceptualisation, data capture, data analysis, first draft preparation, manuscript revision and approval of final manuscript. MB contributed to data analysis, first draft preparation, manuscript revision and approval of final manuscript. SJ contributed to data capture and approval of final manuscript. MvH contributed to data capture and approval of final manuscript. NlR contributed to data capture and approval of final manuscript. MG contributed to data capture and approval of final manuscript. SvdM contributed to data capture and approval of final manuscript. NF contributed to study conceptualisation, data analysis, first draft preparation, manuscript revision and approval of final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The authors declare that this submission is in accordance with the principles laid down by the Responsible Research Publication Position Statements as developed at the 2nd World Conference on Research Integrity in Singapore, 2010. Ethical approval for this study was obtained from the Stellenbosch University Ethics Committee, N18/10/125 prior to the commencement of data collection. All procedures were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008.
Consent to participate
As this is a retrospective study reviewing patient records, a waiver of consent was requested and granted by the Stellenbosch University Ethics Committee.
Consent to publish
I, Dr Obakeng Patial Makhubalo, give my consent for the publication of this manuscript, in its entirety, in the International Orthopaedics journal.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Makhubalo, O., Burger, M., Jakoet, S. et al. Early outcomes of surgically managed civilian gunshot femur fractures at a level one trauma unit in Cape Town, South Africa: a retrospective review. Eur J Trauma Emerg Surg 49, 859–865 (2023). https://doi.org/10.1007/s00068-022-02138-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-022-02138-z