Abstract
Background
Recent research indicates long-term survival benefits of minimally invasive esophagectomy (MIE) compared with open esophagectomy (OE) for patients with esophageal and gastroesophageal junction (GEJ) cancers, but there is a need for more population-based studies.
Methods
We conducted a prospective population-based nationwide cohort study including all patients in Sweden diagnosed with esophageal or junctional cancer who underwent a transthoracic esophagectomy with intrathoracic anastomosis. Data were collected from the Swedish National Register for Esophageal and Gastric Cancer in 2006–2019. Patients were grouped into OE and MIE including hybrid MIE (HMIE) and totally MIE (TMIE). Overall survival and short-term postoperative outcomes were compared using Cox regression and logistic regression models, respectively. All models were adjusted for age, sex, American Society of Anesthesiologists (ASA) score, clinical T and N stage, neoadjuvant therapy, year of surgery, and hospital volume.
Results
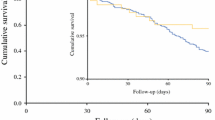
Among 1404 patients, 998 (71.1%) underwent OE and 406 (28.9%) underwent MIE. Compared with OE, overall survival was better following MIE (hazard ratio [HR] 0.72, 95% confidence interval [CI] 0.55–0.94), TMIE (HR 0.67, 95% CI 0.47–0.94), and possibly also after HMIE (HR 0.76, 95% CI 0.56–1.02). MIE was associated with shorter operation time, less intraoperative bleeding, higher number of resected lymph nodes, and shorter hospital stay compared with OE. MIE was also associated with fewer overall complications (odds ratio [OR] 0.70, 95% CI 0.47–1.03) as well as non-surgical complications (OR 0.64, 95% CI 0.40–1.00).
Conclusions
MIE seems to offer better survival and similar or improved short-term postoperative outcomes in esophageal and GEJ cancers compared with OE in this unselected population-based cohort.


Similar content being viewed by others
References
Fitzmaurice C, Abate D, Abbasi N, et al. Global, regional, and national cancer incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life-years for 29 cancer groups, 1990 to 2017: a systematic analysis for the global burden of disease study. JAMA Oncol. 2019;5(12):1749–68.
Sjoquist KM, Burmeister BH, Smithers BM, et al. Survival after neoadjuvant chemotherapy or chemoradiotherapy for resectable oesophageal carcinoma: an updated meta-analysis. Lancet Oncol. 2011;12(7):681–92.
van Hagen P, Hulshof MC, van Lanschot JJ, et al. Preoperative chemoradiotherapy for esophageal or junctional cancer. N Engl J Med. 2012;366(22):2074–84.
Low DE, Kuppusamy MK, Alderson D, et al. Benchmarking complications associated with esophagectomy. Ann Surg. 2019;269(2):291–8.
Biere SS, van Berge Henegouwen MI, Maas KW, et al. Minimally invasive versus open oesophagectomy for patients with oesophageal cancer: a multicentre, open-label, randomised controlled trial. Lancet. 2012;379:1887–92.
Mariette C, Markar SR, Dabakuyo-Yonli TS, et al. Hybrid minimally invasive esophagectomy for esophageal cancer. N Engl J Med. 2019;380(2):152–62.
Maas KW, Cuesta MA, van Berge Henegouwen MI, et al. Quality of life and late complications after minimally invasive compared to open esophagectomy: results of a randomized trial. World J Surg. 2015;39(8):1986–93.
Straatman J, van der Wielen N, Cuesta MA, et al. Minimally invasive versus open esophageal resection. Ann Surg. 2017;266(2):232–6.
van der Sluis PC, van der Horst S, May AM, et al. Robot-assisted minimally invasive thoracolaparoscopic esophagectomy versus open transthoracic esophagectomy for resectable esophageal cancer: a randomized controlled trial. Ann Surg. 2019;269(4):621–30.
Mariette C, Markar S, Dabakuyo-Yonli TS, et al. Health-related quality of life following hybrid minimally invasive versus open esophagectomy for patients with esophageal cancer, analysis of a multicenter, open-label, randomized phase III controlled trial: the MIRO trial. Ann Surg. 2020;271(6):1023–9.
Markar SR, Ni M, Gisbertz SS, et al. Implementation of minimally invasive esophagectomy from a randomized controlled trial setting to national practice. J Clin Oncol. 2020;38(19):2130–9.
Mamidanna R, Bottle A, Aylin P, Faiz O, Hanna GB. Short-term outcomes following open versus minimally invasive esophagectomy for cancer in England: a population-based national study. Ann Surg. 2012;255(2):197–203.
Takeuchi H, Miyata H, Gotoh M, et al. A risk model for esophagectomy using data of 5354 patients included in a Japanese nationwide web-based database. Ann Surg. 2014;260(2):259–66.
Sihag S, Kosinski AS, Gaissert HA, Wright CD, Schipper PH. Minimally invasive versus open esophagectomy for esophageal cancer: a comparison of early surgical outcomes from The Society of Thoracic Surgeons National Database. Ann Thorac Surg. 2016;101(4):1281–8 (discussion 1288-1289).
Seesing MFJ, Gisbertz SS, Goense L, et al. A propensity score matched analysis of open versus minimally invasive transthoracic esophagectomy in The Netherlands. Ann Surg. 2017;266(5):839–46.
Gottlieb-Vedi E, Kauppila JH, Malietzis G, Nilsson M, Markar SR, Lagergren J. Long-term survival in esophageal cancer after minimally invasive compared to open esophagectomy: a systematic review and meta-analysis. Ann Surg. 2019;270(6):1005–17.
Gottlieb-Vedi E, Kauppila JH, Mattsson F, et al. Long-term survival in esophageal cancer after minimally invasive esophagectomy compared to open esophagectomy. Ann Surg. 2021. https://doi.org/10.1097/SLA.0000000000004645.
Ludvigsson JF, Almqvist C, Bonamy AK, et al. Registers of the Swedish total population and their use in medical research. Eur J Epidemiol. 2016;31(2):125–36.
Vandenbroucke JP, von Elm E, Altman DG, et al. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): explanation and elaboration. Int J Surg. 2014;12(12):1500–24.
Linder G, Lindblad M, Djerf P, et al. Validation of data quality in the Swedish National Register for Oesophageal and Gastric Cancer. Br J Surg. 2016;103(10):1326–35.
Buuren SV, Groothuis-Oudshoorn K. mice: Multivariate imputation by chained equations in R. J Stat Softw. 2011;45(3):1–67.
Grambsch PM, Therneau TM. Proportional hazards tests and diagnostics based on weighted residuals. Biometrika. 1994;81(3):515–26.
Lake A, Williams E. ASA classification and perioperative variables: graded anaesthesia score? Br J Anaesth. 1997;78:228–9.
Brierley JD, Gospodarowicz MK, Wittekind C. Oesophagus and oesophagogastric junction. In: J Brierley, M Gospodarowicz, C Wittekind, editors. TNM classification of malignant tumours. 8th edn. Oxford, Hoboken: Wiley; 2017. p. 57–62.
Rice TW, Patil DT, Blackstone EH. 8th edition AJCC/UICC staging of cancers of the esophagus and esophagogastric junction: application to clinical practice. Ann Cardiothorac Surg. 2017;6(2):119–30.
Henneman D, Dikken JL, Putter H, et al. Centralization of esophagectomy: how far should we go? Ann Surg Oncol. 2014;21(13):4068–74.
Therneau TM, Crowson CS, Atkinson EJ. Adjusted survival curves. 2015. Available at https://cran.r-project.org/web/packages/survival/vignettes/adjcurve.pdf.
Sakamoto T, Fujiogi M, Matsui H, Fushimi K, Yasunaga H. Comparing perioperative mortality and morbidity of minimally invasive esophagectomy versus open esophagectomy for esophageal cancer: a nationwide retrospective analysis. Ann Surg. 2021;274(2):324–30.
Yerokun BA, Sun Z, Yang CJ, et al. Minimally invasive versus open esophagectomy for esophageal cancer: a population-based analysis. Ann Thorac Surg. 2016;102(2):416–23.
Kalff MC, Fransen LFC, de Groot EM, et al. Long-term survival after minimally invasive versus open esophagectomy for esophageal cancer: a nationwide propensity-score matched analysis. Ann Surg. 2020. https://doi.org/10.1097/SLA.0000000000004708.
Fransen LFC, Berkelmans GHK, Asti E, et al. The effect of postoperative complications after minimally invasive esophagectomy on long-term survival: an international multicenter cohort study. Ann Surg. 2021;274(6):e1129–37.
Lerut T, Moons J, Coosemans W, et al. Postoperative complications after transthoracic esophagectomy for cancer of the esophagus and gastroesophageal junction are correlated with early cancer recurrence: role of systematic grading of complications using the modified Clavien classification. Ann Surg. 2009;250(5):798–807.
van der Schaaf M, Derogar M, Johar A, et al. Reoperation after oesophageal cancer surgery in relation to long-term survival: a population-based cohort study. BMJ Open. 2014;4(3):e004648.
Maas KW, Biere SS, van Hoogstraten IM, van der Peet DL, Cuesta MA. Immunological changes after minimally invasive or conventional esophageal resection for cancer: a randomized trial. World J Surg. 2014;38(1):131–7.
Yamashita K, Watanabe M, Mine S, et al. Minimally invasive esophagectomy attenuates the postoperative inflammatory response and improves survival compared with open esophagectomy in patients with esophageal cancer: a propensity score matched analysis. Surg Endosc. 2018;32(11):4443–50.
Kauppila JH, Xie S, Johar A, Markar SR, Lagergren P. Meta-analysis of health-related quality of life after minimally invasive versus open oesophagectomy for oesophageal cancer. Brit J Surg. 2017;104(9):1131–40.
Visser E, Markar SR, Ruurda JP, Hanna GB, van Hillegersberg R. Prognostic value of lymph node yield on overall survival in esophageal cancer patients: a systematic review and meta-analysis. Ann Surg. 2019;269(2):261–8.
Klevebro F, Scandavini CM, Kamiya S, Nilsson M, Lundell L, Rouvelas I. Single center consecutive series cohort study of minimally invasive versus open resection for cancer in the esophagus or gastroesophageal junction. Dis Esophagus. 2018;31(10):doy027.
Linder G, Jestin C, Sundbom M, Hedberg J. Safe introduction of minimally invasive esophagectomy at a medium volume center. Scand J Surg. 2020;109(2):121–6.
Birkmeyer JD, Siewers AE, Finlayson EV, et al. Hospital volume and surgical mortality in the United States. N Engl J Med. 2002;346(15):1128–37.
Sheetz KH, Dimick JB, Nathan H. Centralization of high-risk cancer surgery within existing hospital systems. J Clin Oncol. 2019;37(34):3234–42.
Markar SR, Karthikesalingam A, Low DE. Enhanced recovery pathways lead to an improvement in postoperative outcomes following esophagectomy: systematic review and pooled analysis. Dis Esophagus. 2015;28(5):468–75.
van Workum F, Stenstra M, Berkelmans GHK, et al. Learning curve and associated morbidity of minimally invasive esophagectomy: a retrospective multicenter study. Ann Surg. 2019;269(1):88–94.
Klevebro F, Alexandersson von Döbeln G, Wang N, et al. A randomized clinical trial of neoadjuvant chemotherapy versus neoadjuvant chemoradiotherapy for cancer of the oesophagus or gastro-oesophageal junction. Ann Oncol. 2016;27(4):660–7.
Funding
No specific funding was received for this work.
Author information
Authors and Affiliations
Contributions
Study design: MH, GL, JH, DE, JJ, JL, LL, ML, MN, and IR. Data analysis: MH and NN. Manuscript writing, review and final approval: all authors.
Corresponding author
Ethics declarations
Disclosures
Masaru Hayami, Nelson Ndegwa, Mats Lindblad, Gustav Linder, Jakob Hedberg, David Edholm, Jan Johansson, Jesper Lagergren, Lars Lundell, Magnus Nilsson, and Ioannis Rouvelas declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hayami, M., Ndegwa, N., Lindblad, M. et al. Population-Based Cohort Study from a Prospective National Registry: Better Long-Term Survival in Esophageal Cancer After Minimally Invasive Compared with Open Transthoracic Esophagectomy. Ann Surg Oncol 29, 5609–5621 (2022). https://doi.org/10.1245/s10434-022-11922-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-11922-5