Abstract
Background
The Burn Specific Health Scale-Brief (BSHS-B) is considered a validated questionnaire to evaluate quality of life after burn. The purpose of this study was to translate the BSHS-B into Spanish and perform its cross-cultural adaptation.
Methods
First, BSHS-B was translated from English into Spanish. Subsequently, 84 patients answered the Spanish version of BSHS-B and SF-36 scales to assess the reliability (Cronbach’s alpha), construct validity (Spearman rank test), and stability in time (intra-class correlation coefficient).
Results
The BSHS-B-Sp showed a good internal consistency with a global Cronbach’s alpha of 0.96. Correlations between the major domains of BSHS-B and SF-36 are reported with Spearman’s coefficient ranging from 0.29 to 0.87 in all sub-domains (p < 0.01). Stability in time was confirmed by intra-class correlation coefficient (0.91–0.99 for every sub-domain and 0.98 for global score, p < 0.001).
Conclusions
The Spanish version of the BSHS-B demonstrated an appropriated internal consistency, construct validity, and stability in time. This fact supports its applicability to evaluate the quality of life of burn patients.
Level of evidence: Not gradable
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Burn injuries cause severe physical and psychological sequelae in patients. It affects their self-esteem, their relationships with family and friends, their body image, and their capacities to work are reduced. These affairs have a vital impact on the quality of life (QoL) of patients.
Quality of life assessment is based on the evaluation of different spheres (physical, social, and psychological). The level of reduction of QoL depends on total body surface area (TBSA) involved and certain critical areas such as hands and head burns, which are especially related in physical and social repercussions, respectively.
QoL questionnaires are absolutely useful for physicians to be aware of the level of satisfaction of patients and establish an adequate approach to improve it. In addition, they help patients to know not only their physical and psychological status, but also their needs and progression. They should be easy to read and understand to facilitate QoL evaluation.
The Burn Specific Health Scale-Brief (BSHS-B) is an extremely useful tool with 40 items. Each item is answered from 0 (total) to 4 (nothing at all). It consists of nine sub-domains: affect, simple abilities, work, interpersonal relationships, heat sensitivity, sexuality, treatment regimens, body image, and hand function [1]. As other quality of life scales, higher scores of BSHS-B refer to better quality of life.
The questionnaire BSHS-B has been translated into French [2], German [3], Italian [4], Chinese [5], Taiwanese [6], Polish [7], Hebrew [8], Persian [9], Norwegian [10], Brazilian [11], Hindi [12], Turkish [13], and Nepali [14].
Although Sanz et al. [15] published the Spanish version of the Burn Specific Health Scale in 1998, any validated Spanish version of the BSHS-B is actually available. Therefore, the purpose of the study was to validate the translated Spanish version of the BSHS-B, and also testing its reliability and validity in clinical practice.
Materials and methods
The study was held by the Plastic and Reconstructive department of a third level hospital in Spain. All patients were informed about the purpose of the study and accepted to participate. Anonymity was maintained during patient inclusion.
The Short-Form 36 Health Survey Questionnaire (SF-36) and the Spanish version of BSHS-B were delivered at the same time to 84 patients who were previously admitted in our institution from January 2015 to December 2020. Both scales were administered by burn surgeons during hospital visits from June 2020 to August 2021.
Inclusion criteria
We included burn patients > 18 years old suffering full thickness burns equal to or larger than 5% of TBSA who underwent surgery or enzymatic debridement.
Exclusion criteria
We excluded pediatric and psychiatric patients, non-Spanish speakers, and patients with a TBSA < 5% or suffering from superficial burns. Dead and lost to follow-up patients between their discharge and the period of the study were also excluded.
Data collection
In total, 222 eligible burn patients were proposed to join the study by phone, but finally, 84 patients accepted. Demographic and clinical data extracted included age, gender, date of admission, percentage of total body surface area (%TBSA), mechanism of burn injury, location of burn, length of stay (LOS), intensive care requirements, surgical procedures, and complications.
Quality of life scales
The Spanish SF-36 questionnaire [16] and the BSHS-B questionnaire [1] that was translated into Spanish (BSHS-B-Sp) were used to investigate the QoL of burn patients.
Short Form 36 Health Survey (SF-36)
The SF-36 was developed by the Medical Outcomes Study (MOS) in 1992 [17] and validated into Spanish in 1995 [16] to measure the general health and QoL. It provides 36 items grouped into 8 domains: (1) Physical functioning, (2) Role physical, (3) Social functioning, (4) Vitality, (5) Bodily pain, (6) General health, (7) Role-emotional, and (8) Mental health. It has already been used to assess the QoL in burn patients in previous studies [2, 4].
Burn Specific Health Scale-Brief (BSHS-B)
The BSHS was created in 1982 in the USA [18] and initially assessed the quality of life through 369 items, later reduced to 114. Subsequently, it was reduced to 80 items (Abbreviated Burn Specific Health Scale, BSHS-A) and then revised by Blalock et al. [19] (Revised Burn Specific Scale, BSHS-R), containing a total of 31 items but it excluded hand function and sexuality.
In 2001, Kildal et al. [1] developed the Burn Specific Health Scale-Brief (BSHS-B) which became one of the most widely used in clinical practice to evaluate QoL in burn patients. It is easy to understand and patients complete it in 10 min approximately. The BSHS-B contains 40 items grouped in 9 sub-domains: heat sensitivity (5 items), work (4 items), simple abilities (3 items), interpersonal relationships (4 items), hand function (5 items), body image (4 items), treatment regimens (5 items), sexuality (3 items), and affect (7 items). Burn patients should score each item on a scale from 0 to 4, where the higher scores, the better quality of life.
Subsequently, Willebrand et al. [20] reported that, with the exception of work sub-domain, all sub-domains can be grouped into 3 internally consistent and well separated domains: affect and relationship domain (interpersonal relationship, sexually, and affect), function domain (hand function and simple abilities), and skin involvement domain (treatment regimens, heat sensitivity, and body image). The work sub-domain can be considered as a separate domain by itself. Mean scores were calculated for the overall scale, for the 3 major domains and for each of the sub-domains.
BSHS-B Spanish version (BSHS-B-Sp)
According to the Scientific Advisory Committee (SAC) of the Medical Outcome Trust (MOT) [21], 3 independent interpreters translated the BSHS-B from the English language into Spanish. Then, we performed a reverse translation from the Spanish version to English by a professional English translator. Not only an adequate translation is enough, but also a cultural adaptation is mandatory, because the different perception of QoL in different countries.
Statistic values
All analyses were performed with the SPSS Statistics 25®. To confirm the reliability of the BSHS-B-Sp, the internal consistency was assessed by Cronbach’s alpha for each sub-domain and the whole instrument. It is considered appropriate when alpha value is above 0.7 [22]. The construct validity of BSHS-B-Sp was determined by the Spearman correlations with the domains of SF-36, which was chosen as the gold standard measure for quality of life.
The stability in time was assessed by the test–retest method and the intra-class correlation coefficient (ICC). The retest was performed at least at 6 months and an ICC ≥ 0.7 is considered acceptable for this purpose.
Results
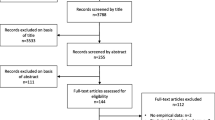
A total of 540 patients were admitted during the years 2015–2020 in our burn unit and 222 met the inclusion criteria. Of these, finally 84 patients accepted to participate in the study and completed both questionnaires (BSHS-B Spanish version and SF-36). The period of time since the date of the burn and the quality of life evaluation was 6–69 months (35.3 ± 17.1 months). Sixteen patients completed the BSHS-B twice to assess stability in time (Fig. 1).
The population of study were 84 patients, mostly men (67.9%), with a mean age of 42 years old (42.88 ± 17.89) and an average total body burn surface area (TBSA) of 23% (23.78 ± 17.43 [range: 5–75%]). Table 1 describes the demographic data of the participants. Flame (n = 65, 77.4%) was the most common mechanism of injury and the 75% of cases were accidental.
Mean and median scores in every domain for the SF-36 questionnaire are described in Table 2.
The BSHS-B-Sp showed a good reliability with a global Cronbach’s alpha of 0.96. In addition, alpha value resulted ≥ 0.7 for every sub-domain, with the higher scores for Simple abilities, Hand function, Body image, and Affect. Table 3 reports alpha values of each domain of the BSHS-B-Sp.
The correlation with SF-36 questionnaire scores allowed to assess the construct validity of BSHS-B. Table 4 reports correlations between the major domains of BSHS-B and SF-36, with Spearman’s coefficient ranging from 0.29 to 0.87, all statistically significant (p < 0.01). Highest correlations were found between sub-domain Affect of the BSHS-B-Sp and Mental Health (0.87), Social Functioning (0.81), Vitality (0.77), and Role-Emotional (0.77) of SF-36.
The stability of the questionnaire in time was determined by intra-class correlation coefficient (ICC). ICC for test–retest ranged between 0.91 to 0.99 and 0.98 for the whole instrument (Table 5).
Patients completed the BSHS-B-Sp questionnaire in 12 min in average (range: 9–15 min).
Relationship between BSHS-B-Sp scores and clinical variables
BSHS-B-Sp and age, gender, and length of stay
Men showed better mean scores in subdomain Affect versus women (19.44 vs 13.78, p < 0.01). A negative correlation between age and subdomain Sexuality (r = − 0.32, p < 0.01) and Simple Abilities (r = − 0.26, p < 0.05) was observed. Length of stay was negatively correlated with subdomain Heat Sensitivity (r = − 0.30, p < 0.01), Simple Abilities (r = − 0.26, p < 0.05), Body Image (r = − 0.23, p < 0.05), and global BSHS-B-Sp (r = − 0.28, p < 0.05).
BSHS-B-Sp and TBSA
TBSA was negatively correlated with global BSHS-B-Sp (r = − 0.24, p < 0.05), Heat Sensitivity (r = − 0.3, p < 0.01), Work (r = − 0.23, p < 0.05), Simple Abilities (r = − 0.24, p < 0.05), and Body image (r = − 0.27, p < 0.05).
BSHS-B-Sp and location of burns
Patients with head and neck burns showed lower mean scores in subdomain Simple Abilities (8.02 vs 10.51, p < 0.01). Patients with upper extremity burns (excluding hands) also showed worse mean scores in subdomain Heat Sensitivity (5.84 vs 9.45, p < 0.05) and Work (8.05 vs 11.40, p < 0.05). In addition, patients with lower extremity burns showed worse mean scores in subdomain Body Image (7.07 vs 10.21, p < 0.05).
Patients with genitalia burns resulted in lower mean scores in global BSHS-B-Sp (55.33 vs 100.98, p < 0.05), Affect (5.87 vs 18.06, p < 0.05), Sexuality (1 vs 8.80, p < 0.01), and Interpersonal Relationships (6.67 vs 14.22, p < 0.01). Patients with abdomen burns showed worse mean scores in subdomain Affect (14.87 vs 19.23, p < 0.05) and Regimens Treatment (9.90 vs 12.87, p < 0.05).
BSHS-B-Sp and burn mechanism and reason
No statistically significant differences were observed between the different mechanisms of burn. However, patients who committed attempts of suicide showed worse mean scores in subdomain Work (Accidental 9.79 ± 5.10, Job accident 6.88 ± 4.68, Suicide attempt 2.25 ± 2.06, p < 0.01), Body Image (Accidental 9.02 ± 5.94, Job accident 5.53 ± 5.71, Suicide attempt 1.75 ± 3.50, p < 0.05), and global BSHS-B-Sp (Accidental 103 ± 37.51, Job accident 97.12 ± 33.29, Suicide attempt 51.25 ± 39.17, p < 0.05).
BSHS-B-Sp and surgery
Burn patients who underwent surgery showed worse mean scores in global BSHS-B-Sp (96.87 vs 126.57, p < 0.05), Affect (16.97 vs 24.71, p < 0.05), Sexuality (8.23 vs 11.71, p < 0.05), and Body Image (7.47 vs 13.43, p < 0.05).
Patients who needed initial escharotomy showed worse mean scores in global BSHS-B-Sp (83.9 vs 108.39, p < 0.01), Heat Sensitivity (3.26 vs 8.72, p < 0.001), Hand Function (12.39 vs 16.09, p < 0.05), Treatment Regimens (9.58 vs 13.06, p < 0.01), Work (6.48 vs 10.23, p < 0.01), and Body Image (5.10 vs 9.64, p < 0.01).
Patients treated with enzymatic debridement (Nexobrid®) showed better mean scores in subdomain Heat Sensitivity (9.93 vs 6.06, p < 0.05) and Body Image (11.79 vs 7.20, p < 0.01).
BSHS-B-Sp and complications
Patients who suffered from any complication during stay showed worse mean scores in global BSHS-B-Sp (90.57 vs 114.35, p < 0.01), Heat Sensitivity (5.08 vs 9.48, p < 0.01), Treatment Regimens (10.74 vs 13.55, p < 0.05), Work (7.66 vs 10.87, p < 0.01), Simple Abilities (8.45 vs 10.58, p < 0.05), and Body Image (6.75 vs 10.03, p < 0.05). Patients with inhalation injury showed worse mean scores in Hand Function (10.63 vs 15.69, p < 0.01) and Simple Abilities (7.06 vs 9.75, p < 0.05).
BSHS-B-Sp and ICU patients
Patients who required intensive care management showed worse mean scores in global BSHS-B-Sp (89.26 vs 107.67, p < 0.05), Heat Sensitivity (4.66 vs 8.39, p < 0.01), Treatment Regimens (9.76 vs 13.43, p < 0.01), Work (7.61 vs 9.87, p < 0.05), and Simple Abilities (7.92 vs 10.33, p < 0.01).
BSHS-B-Sp and job activity
Retired people showed the lowest score in subdomain Sexuality in comparison with other groups (Unemployed 12 ± 0, Student 12 ± 0, Physical work 8.81 ± 4.53, Administrative work 9.92 ± 3.40, Retired/Pensioner 6.12 ± 4.49), statistically significant (p < 0.05).
Discussion
Although the BSHS complete version was validated to Spanish in 1998 [15], it is not available any Spanish validation of the BSHS-B at this moment. It allows plastic surgeons to assess the quality of life of burn patients in Spanish-speaking population in routine clinical practice (in 12 min approximately).
Reliability, construct validity, and stability in time analysis
The Cronbach’s alpha score of the whole instrument (0.96) showed good internal consistency, similarly to previous studies in this field as French (0.93), Italian (0.89), or Chinese (0.97). Every sub-domain obtained at least an alpha value of 0.7 (range 0.70–0.95) as recommended in other publications of the BSHS-B translations [1,2,3,4, 23].
Four sub-domains resulted Cronbach’s alpha values ≥ 0.93 (Hand function, Simple abilities, Body image, and Affect), suggesting a remarkable rate for internal consistency. However, the lowest alpha value was found in the Work sub-domain (0.70).
Correlations with the SF-36 questionnaire were very useful to investigate construct validity. The BSHS-B-Sp shows good correlations with SF-36 and excellent construct validity. Highest correlations were found between Affect of the BSHS-B-Sp and Mental Health and Social Functioning of the SF-36. As mentioned, physical and psychological dysfunction decrease QoL of patients.
Test–retest reliability has been used in other translations to confirm the stability in time of BSHS-B. Our questionnaire showed high global ICC value of 0.98, resulting in good stability in time. French, Persian, and Hebrew versions presented similar results [2, 8, 9].
Subdomains of BSHS-B-Sp analysis
Global BSHS-B-Sp
Length of stay, TBSA, genitalia burns, suicide attempts, surgery necessity, initial escharotomy, complications, and intensive care management have a negative influence on global BSHS-B-Sp scores. These characteristics increase morbidity and have been discussed in the literature [1]. Depression and pain related to anxiety have also a negative impact on quality of life scales [24].
Heat sensitivity
Length of stay, TBSA, upper extremity burns, initial escharotomy, complications, and intensive care management are related to lower scores in subdomain Heat Sensitivity. However, enzymatic debridement is related to better scores, which is according to the literature[25].
Affect
Genitalia and abdomen burns and surgery necessity are associated with lower scores in subdomain Affect. In contrast, male gender is associated with better scores.
Hand function
Initial escharotomy and inhalation injury are associated with lower scores in this subdomain. However, people with hand burns did not show statistically differences, as other studies [24].
Treatment regimens
Initial escharotomy, abdomen burns, complications, and intensive care management are related to lower scores in this subdomain.
Work
TBSA, upper extremity burns, suicide attempts, initial escharotomy, complications, and intensive care management have a negative impact on subdomain Work scores. Dyster et al. [26] showed that returning to work depends on burns severity and type of personality. Those who did not return to work have lower quality of life scores and poor physical and psychological health [27].
Sexuality
Genitalia burns, age, being retired/pensioner and surgery necessity are related to lower scores in this subdomain. The physiological decline of sexual desire in old and retired people could explain these findings.
Interpersonal relationships
Only genitalia burns were associated to lower scores in Interpersonal Relationships. Surprisingly, head and neck burns were not associated to worse scores in this subdomain.
Simple abilities
Length of stay, TBSA, head and neck burns, inhalation injury, complications, and intensive care management are related to worse scores in subdomain Simple Abilities.
Body image
Length of stay, TBSA, lower extremity burns, suicide attempts, surgery necessity, initial escharotomy, and complications are associated with lower scores in this subdomain. However, enzymatic debridement is associated to better results in Body Image.
Limitations
Limitations of the current study must be considered. This study was conducted in one institution and retest method was completed on 16 patients. Nevertheless, the good scores in relation with internal consistency and construct validity make possible to use the BSHS-B Spanish version in clinical practice.
Conclusions
The BSHS-B-Sp reports good results in relation with reliability, construct validity, and stability in time, supporting its application to determine the QoL of burn patients. The use of quality of life questionnaires should be implemented routinely to achieve good results and multidisciplinary approach.
Abbreviations
- BSHS-B:
-
Burn Specific Health Scale-Brief
- BSHS-A:
-
Abbreviated burn specific health scale
- BSHS-R:
-
Revised burn specific scale
- ICC:
-
Intra-class correlation coefficient
- ICU:
-
Intensive care unit
- LOS:
-
Length of stay
- MOT:
-
Medical outcome trust
- TBSA:
-
Total body surface area
- SAC:
-
Scientific Advisory Committee
- SF-36:
-
Short-Form 36 Health Survey Questionnaire
- QoL:
-
Quality of Life
References
Kildal M, Andersson G, Fugl-Meyer AR, Lannerstam K, Gerdin B. Development of a brief version of the Burn Specific Health Scale (BSHS-B). J Trauma Inj Infect Crit Care [Internet]. 2001 Oct;51(4):740–6. Available from: http://journals.lww.com/00005373-200110000-00020
Gandolfi S, Auquit-Auckbur I, Panunzi S, Mici E, Grolleau J-L, Chaput B. Validation of the French version of the Burn Specific Health Scale-Brief (BSHS-B) questionnaire. Burns [Internet]. 2016 Nov;42(7):1573–80. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417916300742
Müller A, Smits D, Jasper S, Berg L, Claes L, Ipaktchi R, et al. Validation of the German version of the Burn Specific Health Scale-Brief (BSHS-B). Burns [Internet]. 2015 Sep;41(6):1333–9. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417915000443
Sideli L, Di Pasquale A, Prestifilippo A, Benigno A, Bartolotta A, Cirrincione CR, et al. Validation of the Italian version of the Burn Specific Health Scale-Brief. Burns [Internet]. 2014 Aug;40(5):995–1000. Available from: https://linkinghub.elsevier.com/retrieve/pii/S030541791300332X
Ling-Juan Z, Jie C, Jian L, Xiao-Ying L, Ping F, Zhao-Fan X, et al. Development of quality of life scale in Chinese burn patients: cross-cultural adaptation process of burn-specific health scale – brief. Burns [Internet]. 2012 Dec;38(8):1216–23. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417912001027
Hwang Y-F, Chen-Sea M-J, Chen C-L, Hsieh C-S. Validation of a Taiwanese version of the Burn-Specific Health Scale-Brief. J Burn Care Res [Internet]. 2016;37(4):e310–6. Available from: https://academic.oup.com/jbcr/article/37/4/e310-e316/4582155
Szczechowicz J, Lewandowski J, Sikorski J. Polish adaptation and validation of Burn Specific Health Scale – brief. Burns [Internet]. 2014 Aug;40(5):1013–8. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417913004075
Stavrou D, Haik J, Wiser I, Winkler E, Liran A, Holloway S, et al. Validation of the Hebrew version of the Burn Specific Health Scale-Brief questionnaire. Burns [Internet]. 2015 Feb;41(1):188–95. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417914001715
Pishnamazi Z, Rejeh N, Heravi-Karimooi M, Vaismoradi M. Validation of the Persian version of the Burn Specific Health Scale – brief. Burns [Internet]. 2013 Feb;39(1):162–7. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417912001428
Litleré Moi A, Wentzel-Larsen T, Salemark L, Hanestad B. Validation of a Norwegian version of the Burn Specific Health Scale. Burns [Internet]. 2003 Sep;29(6):563–70. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417903001463
Piccolo MS, Gragnani A, Daher RP, Scanavino MDT, Brito MJ De, Ferreira LM. Validation of the Brazilian version of the Burn Specific Health Scale-Brief (BSHS-B-Br). Burns [Internet]. 2015 Nov;41(7):1579–86. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417915001278
Mulay AM, Ahuja A, Ahuja RB. Modification, cultural adaptation and validation of burn specific health scale-brief (BSHS-B) for Hindi speaking population. Burns [Internet]. 2015 Nov;41(7):1543–9. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417915001370
Adam M, Leblebici B, Tarim MA, Yildirim S, Bagis S, Akman MN, et al. Validation of a Turkish version of the burn-specific health scale. J Burn Care Res [Internet]. 2009;30(2):288–91; discussion 292–3. Available from: http://www.ncbi.nlm.nih.gov/pubmed/19165114
Shakya R, Manandhar M, Dangol R, Shrestha A. Cross cultural adaptation and validation of burn specific health scale- brief in Nepali (BSHS-B-Np). J Patient-Reported Outcomes [Internet]. 2020 Dec 22;4(1):25. Available from: https://jpro.springeropen.com/articles/https://doi.org/10.1186/s41687-020-00190-0
Salvador Sanz JF, Sanchez-Payá J, Rodriguez Marín J. Spanish version of the Burn-Specific Health Scale. J Trauma [Internet]. 1998 Sep;45(3):581–7. Available from: http://www.ncbi.nlm.nih.gov/pubmed/9751555
Alonso J, Prieto L, Antó JM. [The Spanish version of the SF-36 Health Survey (the SF-36 health questionnaire): an instrument for measuring clinical results]. Med Clin (Barc) [Internet]. 1995 May 27;104(20):771–6. Available from: http://www.ncbi.nlm.nih.gov/pubmed/7783470
Ware JE, Sherbourne CD. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care [Internet]. 1992 Jun;30(6):473–83. Available from: http://www.ncbi.nlm.nih.gov/pubmed/1593914
Blades B, Mellis N, Munster AM. A burn specific health scale. J Trauma [Internet]. 1982 Oct;22(10):872–5. Available from: http://www.ncbi.nlm.nih.gov/pubmed/7131607
Blalock SJ, Bunker BJ, DeVellis RF. Measuring health status among survivors of burn injury: revisions of the Burn Specific Health Scale. J Trauma [Internet]. 1994 Apr;36(4):508–15. Available from: http://www.ncbi.nlm.nih.gov/pubmed/8158712
Willebrand M, Kildal M. A simplified domain structure of the Burn-Specific Health Scale-Brief (BSHS-B): a tool to improve its value in routine clinical work. J Trauma [Internet]. 2008 Jun;64(6):1581–6. Available from: http://www.ncbi.nlm.nih.gov/pubmed/18545127
Aaronson N, Alonso J, Burnam A, Lohr KN, Patrick DL, Perrin E, et al. Assessing health status and quality-of-life instruments: attributes and review criteria. Qual Life Res [Internet]. 2002 May;11(3):193–205. Available from: http://www.ncbi.nlm.nih.gov/pubmed/12074258
Bland JM, Altman DG. Statistics notes: Cronbach’s alpha. BMJ [Internet]. 1997 Feb 22;314(7080):572–572. Available from: https://www.bmj.com/lookup/doi/https://doi.org/10.1136/bmj.314.7080.572
Li D-W, Liu W-Q, Wang H-M, Ying-Sun, Cui L, Zhao F-F. The Chinese language version of the abbreviated Burn Specific Health Scale: a validation study. Burns [Internet]. 2014 Aug;40(5):1001–6. Available from: https://linkinghub.elsevier.com/retrieve/pii/S0305417913003549
van Loey NE, van Beeck EF, Faber BW, van de Schoot R, Bremer M. Health-related quality of life after burns. J Trauma Acute Care Surg [Internet]. 2012 Feb;72(2):513–20. Available from: https://journals.lww.com/01586154-201202000-00029
Hirche C, Kreken Almeland S, Dheansa B, Fuchs P, Governa M, Hoeksema H, et al. Eschar removal by bromelain based enzymatic debridement (Nexobrid®) in burns: European consensus guidelines update. Burns. 2020;46(4).
Dyster-Aas J, Kildal M, Willebrand M, Gerdin B, Ekselius L. Work status and burn specific health after work-related burn injury. Burns. 2004;
Meerding WJ, Looman CWN, Essink-Bot M-L, Toet H, Mulder S, van Beeck EF. Distribution and determinants of health and work status in a comprehensive population of injury patients. J Trauma Inj Infect Crit Care [Internet]. 2004 Jan;56(1):150–61. Available from: http://journals.lww.com/00005373-200401000-00025
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Andalusian Healthcare System. The ethics committee code is 2680-N-20.
Consent to participate
Patients provided written consent to participate in the study as well as to share their data.
Conflict of interest
Antonio García-Díaz, Purificación Gacto-Sánchez, Antonio José Durán-Romero, Alejandro Ruiz-Moya, Julia Molina-Morales, Salvador Carrasco-García, Tomás Gómez-Cía, and José-Juan Pereyra-Rodríguezno declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix. BSHS-B Spanish version (BSHS-B-Sp)
ESCALA DE SALUD ESPECÍFICA DEL PACIENTE QUEMADO (VERSIÓN BREVE)
A continuación se muestra un cuestionario para evaluar la calidad de vida del paciente quemado. Esta información nos permitirá saber cómo se sienten cada día. Si no está seguro de su respuesta, elija la que se parezca más a su situación actual, siendo el valor 0 el máximo (totalmente de acuerdo) y el valor 4 el mínimo (nada de acuerdo).
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
García-Díaz, A., Gacto-Sánchez, P., Durán-Romero, A.J. et al. Validation of the Spanish version of the Burn Specific Health Scale-Brief (BSHS-B) questionnaire. Eur J Plast Surg 45, 809–817 (2022). https://doi.org/10.1007/s00238-022-01954-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-022-01954-1