Abstract
Background and Aim
The aim of the present study is to evaluate a new index (PECS (PsECogSii)index) influenced by PS ECOG and systemic immune-inflammation index (SII) in unresectable locally advanced or metastatic BTC patients treated with first-line chemotherapy.
Methods
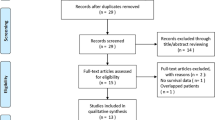
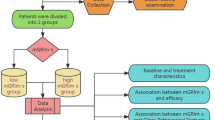
This multicenter, international, study was conducted on a training cohort of 130 patients and in three European and Korean validation cohorts The PECS index was calculated as ECOG × SII index (neutrophil count × platelet count/lymphocyte count). Event-time distributions were estimated using the Kaplan–Meier method and survival curves were compared using the log-rank test.
Results
In the training cohort, the median overall survival (mOS) was 13.2 months, 8.7 months, and 3.8 months for patients with PECS-0, PECS-1, and PECS-2, respectively (PECS-0: HR = 1; PECS-1: HR 1.41; PECS-2: HR 3.23) (p < 0.0001). In the first validation cohort, the mOS was 12.8 months, 10.1 months, and 5.3 months for patients with PECS-0, PECS-1, and PECS-2, respectively (PECS-0: HR = 1; PECS-1: HR 1.29; PECS-2: HR 2.40) (p < 0.0001). In the second validation cohort, the mOS was 21.2 months, 10.2 months, and 3.0 months for patients with PECS-0, PECS-1, and PECS-2, respectively (PECS-0: HR = 1; PECS-1: HR 2.25; PECS-2: HR 9.00) (p < 0.0001). In the third validation cohort, the median OS was 15.5 months, 7.5 months, and 3.7 months for patients with PECS-0, PECS-1, and PECS-2, respectively (PECS-0: ref HR = 1; PECS-1: HR 2.14; PECS-2: HR 5.00) (p < 0.0001). Multivariate analysis in all cohorts confirmed the PECS index as an independent prognostic factor for OS.
Conclusions
The easy assessment, low cost, and reproducibility make PECS index a promising tool to assess the prognosis of BTC patients in future clinical practice.


Similar content being viewed by others
Availability of Data and Materials
On request.
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2019. CA Cancer J Clin. 2019;69(1):7–34.
Hyder O, Hatzaras I, Sotiropoulos GC, et al. Recurrence after operative management of intrahepatic cholangiocarcinoma. Surgery. 2013;153(6):811–8.
Zhang XF, Beal EW, Bagante F, et al. Early versus late recurrence of intrahepatic cholangiocarcinoma after resection with curative intent. Br J Surg. 2018;105(7):848–56.
Valle J, Wasan H, Palmer DH, et al. Cisplatin plus gemcitabine versus gemcitabine for biliary tract cancer. N Engl J Med. 2010;362(14):1273–81.
Kim BJ, Hyung J, Yoo C, et al. Prognostic factors in patients with advanced biliary tract cancer treated with first-line gemcitabine plus cisplatin: retrospective analysis of 740 patients. Cancer Chemother Pharmacol. 2017a;80(1):209–15.
Park HS, Park JS, Chun YJ, et al. Prognostic factors and scoring model for survival in metastatic biliary tract cancer. Cancer Res Treat. 2017;49(4):1127–39.
McNamara MG, Templeton AJ, Maganti M, et al. Neutrophil/lymphocyte ratio as a prognostic factor in biliary tract cancer. Eur J Cancer. 2014a;50(9):1581–9.
Faloppi L, Del Prete M, Casadei Gardini A, et al. The correlation between LDH serum levels and clinical outcome in advanced biliary tract cancer patients treated with first line chemotherapy. Sci Rep. 2016;6:24136.
Park I, Lee JL, Ryu MH, et al. Prognostic factors and predictive model in patients with advanced biliary tract adenocarcinoma receiving first-line palliative chemotherapy. Cancer. 2009a;115(18):4148–55.
Suzuki Y, Kan M, Kimura G, et al. Predictive factors of the treatment outcome in patients with advanced biliary tract cancer receiving gemcitabine plus cisplatin as first-line chemotherapy. J Gastroenterol. 2019;54(3):281–90.
Salati M, Filippi R, Vivaldi C, et al. The prognostic nutritional index predicts survival and response to first-line chemotherapy in advanced biliary cancer [published online ahead of print, 2019 Nov 27]. Liver Int. 2019;https://doi.org/10.1111/liv.14314.
Peixoto RD, Renouf D, Lim H. A population based analysis of prognostic factors in advanced biliary tract cancer. J Gastrointest Oncol. 2014a;5(6):428–32.
Bridgewater J, Lopes A, Wasan H, et al. Prognostic factors for progression-free and overall survival in advanced biliary tract cancer. Ann Oncol. 2016a;27(1):134–40.
Fornaro L, Cereda S, Aprile G, et al. Multivariate prognostic factors analysis for second-line chemotherapy in advanced biliary tract cancer. Br J Cancer. 2014a;110(9):2165–9.
Grivennikov SI, Greten FR, Karin M. Immunity, inflammation, and cancer. Cell. 2010;140(6):883–99.
Duffy AG, Makarova-Rusher OV, Greten TF. The case for immune-based approaches in biliary tract carcinoma. Hepatology. 2016;64(5):1785–91.
Cools-Lartigue J, Spicer J, McDonald B, et al. Neutrophil extracellular traps sequester circulating tumor cells and promote metastasis [published online ahead of print, 2013 Jul 1]. J Clin Invest. 2013;123(8):3446–3458.
Labelle M, Begum S, Hynes RO. Direct signaling between platelets and cancer cells induces an epithelial-mesenchymal-like transition and promotes metastasis. Cancer Cell. 2011a;20(5):576–90.
Mantovani A, Allavena P, Sica A, Balkwill F. Cancer-related inflammation. Nature. 2008a;454(7203):436–44.
Casadei Gardini A, Scarpi E, Faloppi L, et al. Immune inflammation indicators and implication for immune modulation strategies in advanced hepatocellular carcinoma patients receiving sorafenib. Oncotarget. 2016a;7(41):67142–9.
Casadei Gardini A, Marisi G, Canale M, et al. Radiofrequency ablation of hepatocellular carcinoma: a meta-analysis of overall survival and recurrence-free survival. Onco Targets Ther. 2018;11:6555–67.
Casadei Gardini A, Foschi FG, Conti F, et al. Immune inflammation indicators and ALBI score to predict liver cancer in HCV-patients treated with direct-acting antivirals. Dig Liver Dis. 2019;51(5):681–8.
Casadei-Gardini A, Montagnani F, Casadei C, et al. Immune inflammation indicators in anal cancer patients treated with concurrent chemoradiation: training and validation cohort with online calculator (ARC: Anal Cancer Response Classifier) [published correction appears in Cancer Manag Res. 2019 Jun 25;11:5123]. Cancer Manag Res. 2019;11:3631–42.
Proctor MJ, McMillan DC, Morrison DS, Fletcher CD, Horgan PG, Clarke SJ. A derived neutrophil to lymphocyte ratio predicts survival in patients with cancer. Br J Cancer. 2012;107(4):695–9.
Templeton AJ, Ace O, McNamara MG, et al. Prognostic role of platelet to lymphocyte ratio in solid tumors: a systematic review and meta-analysis. Cancer Epidemiol Biomarkers Prev. 2014;23(7):1204–12.
Templeton AJ, McNamara MG, Šeruga B, et al. Prognostic role of neutrophil-to-lymphocyte ratio in solid tumors: a systematic review and meta-analysis. J Natl Cancer Inst. 2014;106(6):dju124.
Gu L, Li H, Chen L, et al. Prognostic role of lymphocyte to monocyte ratio for patients with cancer: evidence from a systematic review and meta-analysis. Oncotarget. 2016;7(22):31926–42.
Geng Y, Shao Y, Zhu D, et al. Systemic immune-inflammation index predicts prognosis of patients with esophageal squamous cell carcinoma: a propensity score-matched analysis . Sci Rep. 2016;6:39482.
Hu B, Yang XR, Xu Y, et al. Systemic immune-inflammation index predicts prognosis of patients after curative resection for hepatocellular carcinoma. Clin Cancer Res. 2014;20(23):6212–22.
Prognostic factors in unresectable biliary tract cancer: a GICO (Gruppo Italiano COlangiocarcinoma) retrospective analysis. Ann Oncol. 2017.
McNamara MG, Templeton AJ, Maganti M, et al. Neutrophil/lymphocyte ratio as a prognostic factor in biliary tract cancer. Eur J Cancer. 2014b;50(9):1581–9.
Peixoto RD, Renouf D, Lim H. A population based analysis of prognostic factors in advanced biliary tract cancer. J Gastrointest Oncol. 2014b;5(6):428–32.
Bridgewater J, Lopes A, Wasan H, et al. Prognostic factors for progression-free and overall survival in advanced biliary tract cancer. Ann Oncol. 2016b;27(1):134–40.
Kim BJ, Hyung J, Yoo C, et al. Prognostic factors in patients with advanced biliary tract cancer treated with first-line gemcitabine plus cisplatin: retrospective analysis of 740 patients. Cancer Chemother Pharmacol. 2017b;80(1):209–15.
Fornaro L, Cereda S, Aprile G, et al. Multivariate prognostic factors analysis for second-line chemotherapy in advanced biliary tract cancer. Br J Cancer. 2014b;110(9):2165–9.
Park I, Lee JL, Ryu MH, et al. Prognostic factors and predictive model in patients with advanced biliary tract adenocarcinoma receiving first-line palliative chemotherapy. Cancer. 2009b;115(18):4148–55.
Bridgewater J, Palmer D, Cunningham D, et al. Outcome of second-line chemotherapy for biliary tract cancer. Eur J Cancer. 2013;49(6):1511.
Cereda S, Belli C, Rognone A, Mazza E, Reni M. Second-line therapy in advanced biliary tract cancer: what should be the standard? Crit Rev Oncol Hematol. 2013;88(2):368–74.
Park HS, Park JS, Chun YJ, et al. Prognostic factors and scoring model for survival in metastatic biliary tract cancer. Cancer Res Treat. 2017;49(4):1127–39.
Casadei Gardini A, Scarpi E, Faloppi L, et al. Immune inflammation indicators and implication for immune modulation strategies in advanced hepatocellular carcinoma patients receiving sorafenib. Oncotarget. 2016b;7(41):67142–9.
Conroy G, Salleron J, Belle A, et al. The prognostic value of inflammation-based scores in advanced hepatocellular carcinoma patients prior to treatment with sorafenib. Oncotarget. 2017;8(56):95853–95864. Published 2017 Sep 30.
Passardi A, Scarpi E, Cavanna L, et al. Inflammatory indexes as predictors of prognosis and bevacizumab efficacy in patients with metastatic colorectal cancer. Oncotarget. 2016;7(22):33210–9.
Wang K, Diao F, Ye Z, et al. Prognostic value of systemic immune-inflammation index in patients with gastric cancer. Chin J Cancer. 2017;36(1):75. Published 2017 Sep 12.
Wang L, Wang C, Wang J, Huang X, Cheng Y. A novel systemic immune-inflammation index predicts survival and quality of life of patients after curative resection for esophageal squamous cell carcinoma. J Cancer Res Clin Oncol. 2017;143(10):2077–86.
Lolli C, Basso U, Derosa L, et al. Systemic immune-inflammation index predicts the clinical outcome in patients with metastatic renal cell cancer treated with sunitinib. Oncotarget. 2016;7(34):54564–71.
Hong X, Cui B, Wang M, Yang Z, Wang L, Xu Q. Systemic immune-inflammation index, based on platelet counts and neutrophil-lymphocyte ratio, is useful for predicting prognosis in small cell lung cancer. Tohoku J Exp Med. 2015;236(4):297–304.
Tong YS, Tan J, Zhou XL, Song YQ, Song YJ. Systemic immune-inflammation index predicting chemoradiation resistance and poor outcome in patients with stage III non-small cell lung cancer. J Transl Med. 2017;15(1):221. Published 2017 Oct 31.
Yu J, Wu X, Yu H, et al. Systemic Immune-inflammation index and circulating T-cell immune index predict outcomes in high-risk acral melanoma patients treated with high-dose interferon. Transl Oncol. 2017;10(5):719–25.
Labelle M, Begum S, Hynes RO. Direct signaling between platelets and cancer cells induces an epithelial-mesenchymal-like transition and promotes metastasis. Cancer Cell. 2011b;20(5):576–90.
Schumacher D, Strilic B, Sivaraj KK, Wettschureck N, Offermanns S. Platelet-derived nucleotides promote tumor-cell transendothelial migration and metastasis via P2Y2 receptor. Cancer Cell. 2013;24(1):130–7.
Gil-Bernabé AM, Ferjancic S, Tlalka M, et al. Recruitment of monocytes/macrophages by tissue factor-mediated coagulation is essential for metastatic cell survival and premetastatic niche establishment in mice. Blood. 2012;119(13):3164–75.
Chen HC, Lin HC, Liu CY, et al. Neutrophil elastase induces IL-8 synthesis by lung epithelial cells via the mitogen-activated protein kinase pathway. J Biomed Sci. 2004;11(1):49–58.
De Larco JE, Wuertz BR, Furcht LT. The potential role of neutrophils in promoting the metastatic phenotype of tumors releasing interleukin-8. Clin Cancer Res. 2004;10(15):4895–900.
Houghton AM, Rzymkiewicz DM, Ji H, et al. Neutrophil elastase-mediated degradation of IRS-1 accelerates lung tumor growth. Nat Med. 2010;16(2):219–23.
Mantovani A, Allavena P, Sica A, Balkwill F. Cancer-related inflammation. Nature. 2008b;454(7203):436–44.
Ha H, Nam AR, Bang JH, et al. Soluble programmed death-ligand 1 (sPDL1) and neutrophil-to-lymphocyte ratio (NLR) predicts survival in advanced biliary tract cancer patients treated with palliative chemotherapy. Oncotarget. 2016 Nov 22.
Author information
Authors and Affiliations
Contributions
Conception and design: A. Casadei Gardini, G Rovesti. Acquisition of data (acquired and managed patients): Giulia Rovesti, Francesco Leone,Giovanni Brandi, Lorenzo Fornaro, Mario Scartozzi, Monica Niger, Changhoon Yoo, Francesco Caputo, Roberto Filippi, Mariaelena Casagrande, Nicola Silvestris, Daniele Santini, Luca Faloppi, Andrea Palloni, Massimo Aglietta, Caterina Vivaldi, Hyungwoo Cho, Eleonora Lai, Elisabetta Fenocchio, Federico Nichetti, Nicoletta Pella, Stefania De Lorenzo, Massimo Di Maio, Enrico Vasile, Filippo de Braud, Jae Ho Jeong, Giuseppe Aprile, Giulia Orsi, Stefano Cascinu, Andrea Casadei-Gardini Analysis and interpretation of data: A. Casadei Gardini, G Rovesti. Writing, review, and/or revision of the manuscript: A. Casadei Gardini, G Rovesti. Final approval of manuscript: All authors.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
Ethical approval All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent Informed consent was obtained from all individual participants included in the study.
Informed Consent
All patients signed the informed consent.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rovesti, G., Leone, F., Brandi, G. et al. Prognostic Role of a New Index Tested in European and Korean Advanced Biliary Tract Cancer Patients: the PECS Index. J Gastrointest Canc 53, 289–298 (2022). https://doi.org/10.1007/s12029-021-00596-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-021-00596-z