Abstract
Objective
We sought to evaluate demographic, clinical, and habits/occupational variables between phenotypic extremes in Parkinson’s disease (PD).
Methods
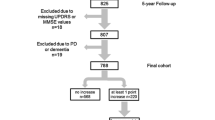
Databases from nine movement disorders centers across seven countries were retrospectively searched for subjects meeting criteria for very slowly progressive, benign, PD (bPD) and rapidly progressive, malignant, PD (mPD). bPD was defined as Hoehn and Yahr (H&Y) stage ≤ 3, normal cognitive function, and Schwab and England (S&E) score ≥ 70 after ≥ 20 years of PD (≥ 10 years if older than 60 at PD onset); mPD as H&Y > 3, S&E score < 70, and cognitive impairment within 10 years from PD onset. We performed between-group analysis of demographic, habits/occupational, and clinical features at baseline and follow-up and unsupervised data-driven analysis of the clinical homogeneity of bPD and mPD.
Results
At onset, bPD subjects (n = 210) were younger, had a single limb affected, lower severity and greater asymmetry of symptoms, and lower prevalence of depression than mPD (n = 155). bPD was associated with active smoking and physical activity, mPD with agricultural occupation. At follow-up, mPD showed higher prevalence of depression, hallucinations, dysautonomia, and REM behaviour disorder. Interestingly, the odds of mPD were significantly reduced by the presence of dyskinesia and wearing-off. Data-driven analysis confirmed the independent clustering of bPD and mPD, with age at onset emerging as a critical discriminant between the two groups (< 46-year-old vs. > 68-year-old).
Conclusions
Phenotypic PD extremes showed distinct demographic, clinical, and habits/occupational factors. Motor complications may be conceived as markers of therapeutic success given their attenuating effects on the odds of mPD.



Similar content being viewed by others

References
Berg D, Postuma RB, Bloem B et al (2014) Time to redefine PD? Introductory statement of the MDS Task Force on the definition of Parkinson's disease. Mov Disord 29:454–462
Hely MA, Reid WG, Adena MA, Halliday GM, Morris JG (2008) The Sydney multicenter study of Parkinson's disease: the inevitability of dementia at 20 years. Mov Disord 23:837–844
Forsaa EB, Larsen JP, Wentzel-Larsen T, Alves G (2010) What predicts mortality in Parkinson disease?: a prospective population-based long-term study. Neurology 75:1270–1276
Schrag A, Schott JM (2006) Epidemiological, clinical, and genetic characteristics of early-onset parkinsonism. Lancet Neurol 5:355–363
Ahlskog JE (2007) Beating a dead horse: dopamine and Parkinson disease. Neurology 69:1701–1711
Kempster PA, O’Sullivan SS, Holton JL, Revesz T, Lees AJ (2010) Relationships between age and late progression of Parkinson’s disease: a clinico-pathological study. Brain 133:1755–1762
Coelho M, Ferreira JJ (2012) Late-stage Parkinson disease. Nat Rev Neurol 8:435–442
Romagnolo A, Fabbri M, Merola A et al (2018) Beyond 35 years of Parkinson's disease: a comprehensive clinical and instrumental assessment. J Neurol 265:1989–1997
Merola A, Zibetti M, Angrisano S et al (2011) Parkinson's disease progression at 30 years: a study of subthalamic deep brain-stimulated patients. Brain 134:2074–2084
Fereshtehnejad SM, Romenets SR, Anang JB, Latreille V, Gagnon JF, Postuma RB (2015) New clinical subtypes of parkinson disease and their longitudinal progression: a prospective cohort comparison with other phenotypes. JAMA Neurol 72:863–873
Erro R, Vitale C, Amboni M et al (2013) The heterogeneity of early Parkinson’s disease: a cluster analysis on newly diagnosed untreated patients. PLoS ONE 8:e70244
Van Rooden SM, Heiser WJ, Kok JN, Verbaan D, van Hilten JJ, Marinus J (2010) The identification of Parkinson's disease subtypes using cluster analysis: a systematic review. Mov Disord 25:969–978
Mestre TA, Eberly S, Tanner C et al (2018) Reproducibility of data-driven Parkinson's disease subtypes for clinical research. Parkinsonism Relat Disord 56:102–106
De Pablo-Fernández E, Lees AJ, Holton JL, Warner TT (2019) Prognosis and neuropathologic correlation of clinical subtypes of Parkinson disease. JAMA Neurol 76:470–479
Pilotto A, Romagnolo A, Tuazon JA et al (2019) Orthostatic hypotension and REM sleep behaviour disorder: impact on clinical outcomes in α-synucleinopathies. J Neurol Neurosurg Psychiatry 90:1257–1263
Postuma RB, Bertrand J-A, Montplaisir J et al (2012) Rapid eye movement sleep behavior disorder and risk of dementia in Parkinson’s disease: a prospective study. Mov Disord 27:720–726
Tanner CM, Goldman SM, Ross GW, Grate SJ (2014) The disease intersection of susceptibility and exposure: chemical exposures and neurodegenerative disease risk. Alzheimers Dement 10:S213–225
Gibb WRG, Lees AJ (1988) The relevance of the Lewy body to the pathogenesis of idiopathic Parkinson’s disease. J Neurol Neurosurg Psychiatry 51:745–752
Nasreddine ZS, Phillips NA, Bédirian V et al (2005) The Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment. J Am Geriatr Soc 53:695–699
Folstein MF, Folstein SE, McHugh PR (1975) "Mini-mental state". A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
Schwab J, England A (1969) Projection technique for evaluating surgey in Parkinson’s disease. In: Gillingham F, Donaldson M (eds) Third symposium on Parkinson’s disease. Churchill Livingstone, Edinburgh, pp 152–157
Miller AR, Trieman DJ, Cain PS, Roos PA (1980) Work, jobs, and occupations: a critical review of the dictionary of occupational titles. National Academy Press, Washington
Fahn S, Elton RL (1987) UPDRS Development Committee. The unified Parkinson’s disease rating scale. In: Fahn S, Marsden CD, Calne DB, Goldstein M (eds) Recent developments in Parkinson’s disease, 2nd edn. Macmillan Health Care Information, Florham Park, pp 153–163
Postuma RB, Arnulf I, Hogl B et al (2012) A single-question screen for rapid eye movement sleep behavior disorder: a multicenter validation study. Mov Disord 27:913–916
Tomlinson CL, Stowe R, Patel S, Rick C, Gray R, Clarke CE (2010) Systematic review of levodopa dose equivalency reporting in Parkinson's disease. Mov Disord 25:2649–2653
Arias-Palencia NM, Solera-Martínez M, Gracia-Marco L et al (2015) Levels and patterns of objectively assessed physical activity and compliance with different public health guidelines in university students. PLoS ONE 10:e0141977
Harris RJ (1985) A primer of multivariate statistics, 2nd edn. Academic Press, New York
Dziak JJ, Lanza ST, Tan X (2014) Effect size, statistical power and sample size requirements for the bootstrap likelihood ratio test in latent class analysis. Struct Equ Modeling 21:534–352
Lewis SJ, Foltynie T, Blackwell AD, Robbins TW, Owen AM, Barker RA (2005) Heterogeneity of Parkinson’s disease in the early clinical stages using a data driven approach. J Neurol Neurosurg Psychiatry 76:343–348
Ascherio A, Schwarzschild MA (2016) The epidemiology of Parkinson’s disease: risk factors and prevention. Lancet Neurol 15:1257–1272
Marras C, Canning CG, Goldman SM (2019) Environment, lifestyle, and Parkinson's disease: Implications for prevention in the next decade. Mov Disord 34:801–811
Hirsch MA, Iyer SS, Sanjak M (2016) Exercise-induced neuroplasticity in human Parkinson's disease: what is the evidence telling us? Parkinsonism Relat Disord 22(Suppl 1):S78–81
Ahmed H, Abushouk AI, Gabr M, Negida A, Abdel-Daim MM (2017) Parkinson's disease and pesticides: a meta-analysis of disease connection and genetic alterations. Biomed Pharmacother 90:638–649
Fitzmaurice AG, Rhodes SL, Cockburn M, Ritz B, Bronstein JM (2014) Aldehyde dehydrogenase variation enhances effect of pesticides associated with Parkinson disease. Neurology 82:419–426
Moisan F, Spinosi J, Delabre L et al (2015) Association of Parkinson's disease and its subtypes with agricultural pesticide exposures in men: a case-control study in France. Environ Health Perspect 123:1123–1129
Calabrese V, Santoro A, Monti D et al (2018) Aging and Parkinson's disease: inflammaging, neuroinflammation and biological remodeling as key factors in pathogenesis. Free Radic Biol Med 115:80–91
de la Fuente-Fernández R, Schulzer M, Kuramoto L et al (2011) Age-specific progression of nigrostriatal dysfunction in Parkinson's disease. Ann Neurol 69:803–810
Brotchie J, Fitzer-Attas C (2009) Mechanisms compensating for dopamine loss in early Parkinson disease. Neurology 72:S32–38
Espay AJ, Lang AE (2020s) Parkinson diseases in the 2020s and beyond: replacing clinico-pathologic convergence with systems biology divergence. J Parkinsons Dis 8:S59–64
Picconi B, Centonze D, Håkansson K et al (2003) Loss of bidirectional striatal synaptic plasticity in l-DOPA-induced dyskinesia. Nat Neurosci 6:501–506
Iravani MM, McCreary AC, Jenner P (2012) Striatal plasticity in Parkinson's disease and l-dopa induced dyskinesia. Parkinsonism Relat Disord 18:S123–125
Espay AJ, Morgante F, Merola A et al (2018) Levodopa-induced dyskinesia in Parkinson disease: current and evolving concepts. Ann Neurol 84:797–811
Kishore A, James P, Krishnan S, Yahia-Cherif L, Meunier S, Popa T (2017) Motor cortex plasticity can indicate vulnerability to motor fluctuation and high L-DOPA need in drug-naïve Parkinson's disease. Parkinsonism Relat Disord 35:55–62
Espay AJ, Lang AE (2017) Common myths in the use of levodopa in Parkinson disease: when clinical trials misinform clinical practice. JAMA Neurol 74:633–634
Verschuur CVM, Suwijn SR, Boel JA et al (2019) Randomized delayed-start trial of levodopa in Parkinson's disease. N Engl J Med 380:315–324
Fasano A, Canning CG, Hausdorff JM, Lord S, Rochester L (2017) Falls in Parkinson’s disease: a complex and evolving picture. Mov Disord 32:1524–1536
Fraigne JJ, Torontali ZA, Snow MB, Peever JH (2015) REM sleep at its core—circuits, neurotransmitters, and pathophysiology. Front Neurol 6:1–9
Del Tredici K, Braak H (2013) Dysfunction of the locus coeruleus—norepinephrine system and related circuitry in Parkinson’s disease-related dementia. J Neurol Neurosurg Psychiatry 84:774–783
Schrag A, Siddiqui UF, Anastasiou Z, Weintraub D, Schott JM (2017) Clinical variables and biomarkers in prediction of cognitive impairment in patients with newly diagnosed Parkinson’s disease: a cohort study. Lancet Neurol 16:66–75
Anang JB, Gagnon JF, Bertrand JA et al (2014) Predictors of dementia in Parkinson disease: a prospective cohort study. Neurology 83:1253–1260
Chaudhuri KR, Martinez-Martin P, Brown RG et al (2007) The metric properties of a novel non-motor symptoms scale for Parkinson's disease: results from an international pilot study. Mov Disord 22:1901–1911
Acknowledgements
Authors acknowledge the contribution of the “Fondazione Grigioni per il Morbo di Parkinson”, Milan, Italy.
Author information
Authors and Affiliations
Contributions
AM: study concept and design, analysis and interpretation of data, drafting/revising the manuscript for content. AR: study concept and design, acquisition and interpretation of data, drafting/revising the manuscript for content. AKD: analysis and interpretation of data, drafting/revising the manuscript for content. AP: interpretation of data, revising the manuscript for content. DB: interpretation of data, revising the manuscript for content. PJG-R: acquisition of data, revising the manuscript for content. MF: acquisition of data, revising the manuscript for content. CAA: acquisition of data, revising the manuscript for content. MZ: acquisition of data, revising the manuscript for content. LL: interpretation of data, revising the manuscript for content. AP: acquisition of data, revising the manuscript for content. SB: acquisition of data, revising the manuscript for content. FM: interpretation of data, revising the manuscript for content. KZ: acquisition of data, revising the manuscript for content. CG: acquisition of data, revising the manuscript for content. ES: interpretation of data, revising the manuscript for content. FR-P: acquisition of data, revising the manuscript for content. MK: interpretation of data, revising the manuscript for content. PT: acquisition of data, revising the manuscript for content. LMO: acquisition of data, revising the manuscript for content. GP: acquisition of data, revising the manuscript for content. ES: acquisition of data, revising the manuscript for content. FDS: acquisition of data, revising the manuscript for content. SB: acquisition of data, revising the manuscript for content. RS: interpretation of data, revising the manuscript for content. RPM: interpretation of data, revising the manuscript for content. RC: interpretation of data, revising the manuscript for content. RC: study concept and design, interpretation of data, revising the manuscript for content. AE: study concept and design, interpretation of data, revising the manuscript for content. All the co-authors listed above gave their final approval of this manuscript version. All the co-authors agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflicts of interest
Dr Merola is supported by NIH (KL2 TR001426) and has received speaker honoraria from CSL Behring, Abbvie, and Cynapsus Therapeutics. He has received grant support from Lundbeck. Dr Romagnolo has received grant support and speaker honoraria from AbbVie, speaker honoraria from Chiesi Farmaceutici and travel grants from Lusofarmaco, Chiesi Farmaceutici, Medtronic, and UCB Pharma. Dr. Dwivedi is supported as a co-investigator by the NIH (1R01HL125016-01), (1 R21 HL143030-01) and (1R21 AI133207) grants and as a collaborator in NIH R21 AI118228 grant. He has been also serving as a statistician in CPRIT grants (PP180003, PP170068, PP170004, PP140164, 140211, PP110156, PP150031, and PP130083), CCTST K12 (consultant) award, Coldwell (co-investigator) and TMF (co-investigator). Dr. Dwivedi is a director of Biostatistics & Epidemiology Consulting Lab at the TTUHSC EP. Dr. Padovani has received grant support from Ministry of Health (MINSAL) and Ministry of Education, Research and University (MIUR), from CARIPLO Foundation; personal compensation as a consultant/scientific advisory board member for Avanir, Lundbeck, Eli-Lilly, Neuraxpharma, Biogen, GE Health. Dr. Berg reports grants from Janssen Pharmaceutica, grants from Damp foundation, grants from German Parkinson’s Disease Association (dPV), grants from BMWi, grants from BMBF, grants from Parkinson Fonds Deutschland GmbH, grants and speaker’s honoraria from and consultancies for UCB Pharma GmbH, grants from Novartis Pharma GmbH, grants and speaker’s honoraria from and consultancies for Lundbeck, speaker’s honoraria from and consultancies for BIAL, grants from the EU, speaker’s honoraria from and consultancies for Biogen, and speaker’s honoraria from AbbVie, Zambon and Desitin. Dr. Garcia-Ruiz has received research support from Allergan and UCB, personal compensation as a consultant/scientific advisory board from Italfarmaco, Britannia, Bial, Zambon, and speaker’s honoraria from Italfarmaco, UCB, Zambon, Allergan and Abbvie. Dr. Fabbri has no financial conflicts to disclose. Dr. Artusi has received travel grants from Zambon and Abbvie. Dr. Zibetti has received honoraria from Medtronic, Zambon Pharma and AbbVie. Dr. Lopiano has received honoraria for lecturing and travel grants from Medtronic, UCB Pharma, and AbbVie. Dr. Pilotto has received speaker honoraria from BioMarin Pharmaceutical, Chiesi Pharmaceuticals, Nutricia Pharmaceuticals, UCB Pharma and Zambon Pharmaceuticals. He received grants from the Italian Ministry of Health, Zambon Italia, Vitaflo Germany. Dr. Bonacina has no financial conflicts to disclose. Dr. Morgante has received speaking honoraria from Medtronic, Zambon, Chiesi, Abbvie, Merz, Bial; personal compensation as a consultant/scientific advisory board member from Merz, Abbvie, Bial, Medtronic. Dr. Zeuner has received research support from an intramural grant from the Christian-Albrechts-University of Kiel, from the Benign Essential Blepharospasm Research Foundation and with an unrestricted grant from Ipsen. She has received lecture fees from Allergan, Merz, AbbVie and Bayer outside the submitted work. She has served as a consultant and received fees from Merz and Ipsen. Dr. Griewin has no financial conflicts to disclose. Dr. Schaeffer has received intramural research funding from the University of Kiel and speaker’s honoraria from Bayer Vital GmbH and Novartis. Dr. Rodriguez-Porcel has no financial conflicts to disclose. Dr. Kauffman is an employee of the CONICET. He has received grant support from Ministry of Science and Technology of Argentina and Ministry of Health of Buenos Aires. He has received honoraria payments for educational activities from Janssen Pharmaceuticals and Bago Pharmaceuticals. Dr. Turcano has no financial conflicts to disclose. Dr. de Oliveira has no financial conflicts to disclose. Dr. Palermo has no financial conflicts to disclose. Ms. Shanks has no financial conflicts to disclose. Dr. Del Sorbo has no financial conflicts to disclose. Dr. Bonvegna has no financial conflicts to disclose. Dr. Savica has received research support from the National Institute on Aging, the National Institute of Neurological Disorders and Stroke, the Mayo Clinic Small Grants Program National Center for Advancing Translational Sciences (NCATS), and unrestricted grant from ACADIA Pharmaceuticals, INC. Dr. Munhoz has no financial conflicts to disclose. Dr. Ceravolo has received fees for speech by Abbvie, General Electric, Zambon, UCB, Lusofarmaco. Dr. Cilia has has received speaking honoraria from Zambon, UCB, Bial; personal compensation as a consultant from Roche. Dr. Espay has received grant support from the NIH, Great Lakes Neurotechnologies and the Michael J Fox Foundation; personal compensation as a consultant/scientific advisory board member for Abbvie, TEVA, Impax, Acadia, Acorda, Intrance, Cynapsus/Sunovion, Lundbeck, and USWorldMeds; publishing royalties from Lippincott Williams & Wilkins, Cambridge University Press, and Springer; and honoraria from Abbvie, UCB, USWorldMeds, Lundbeck, Acadia, the American Academy of Neurology, and the Movement Disorders Society.
Ethical approval
The study received IRB/ethics committee approval at all participating centers and was conducted in accordance with the Good Clinical Practice and the International Conference on Harmonization guidelines and any applicable national and local regulations. The authors declare that they acted in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Merola, A., Romagnolo, A., Dwivedi, A.K. et al. Benign versus malignant Parkinson disease: the unexpected silver lining of motor complications. J Neurol 267, 2949–2960 (2020). https://doi.org/10.1007/s00415-020-09954-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-020-09954-6